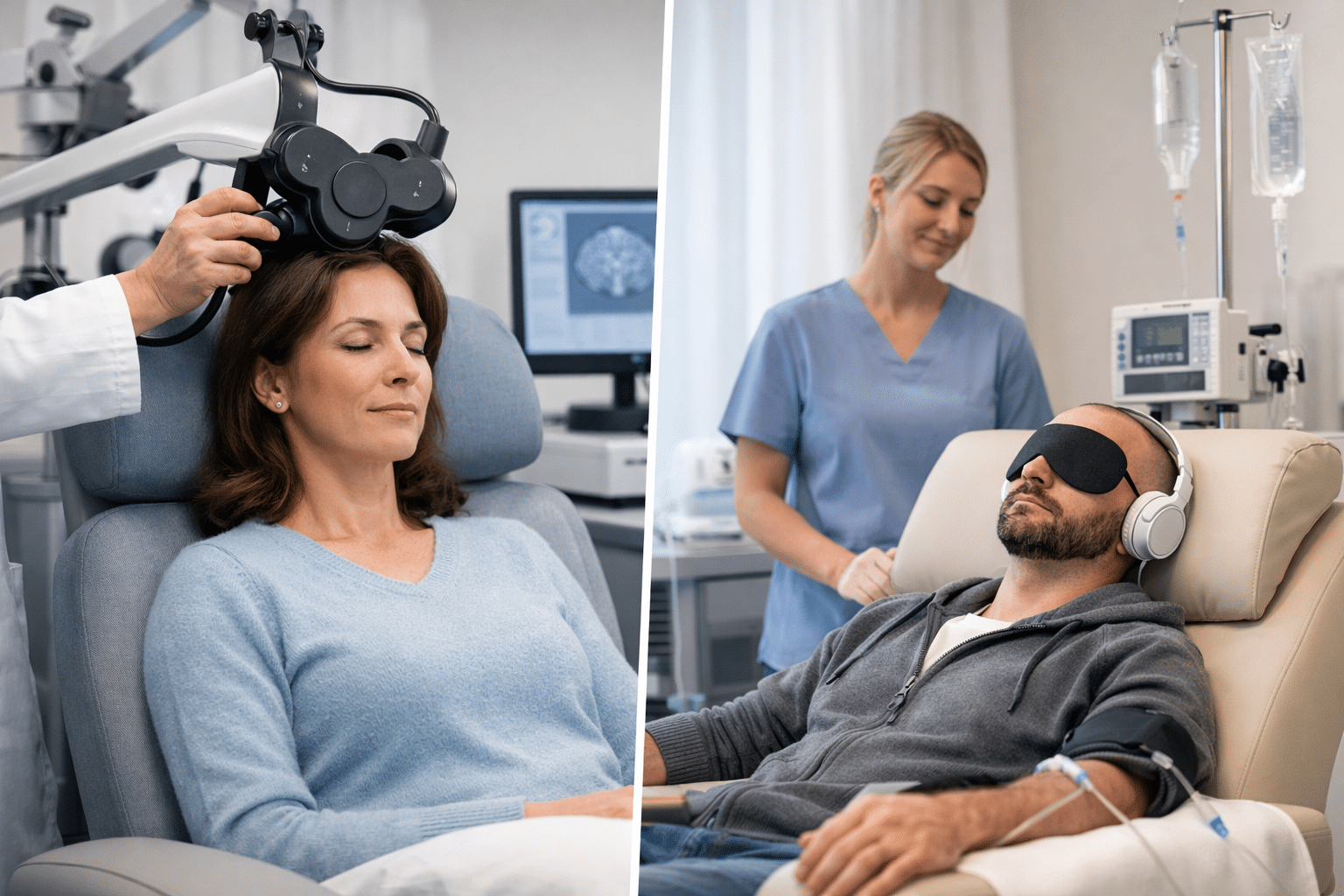
Finding effective depression treatment isn’t always straightforward. For some people, medication works, and that’s the end of the story. For others, the journey looks more like a series of adjustments: different medications, different doses, and sometimes different approaches entirely. That’s not a sign of failure. It’s how treatment works for a lot of people.
This article walks through how psychiatric treatment plans evolve, why some patients don’t get the relief they’re looking for from initial options, and how clinicians think through the decision to introduce something like TMS therapy.
Quick Answer Summary
TMS therapy is typically recommended after first-line depression treatments, such as antidepressants and psychotherapy, have not provided sufficient relief. Clinicians consider factors like treatment history, symptom severity, side effects, and patient goals before introducing TMS. Because it works through a different mechanism than medication, TMS offers an effective next step for patients with treatment-resistant depression and is often integrated into a broader psychiatric care plan.
The Evolution of a Psychiatric Treatment Plan
Psychiatric treatment for depression usually starts in a predictable place. Clinicians typically open with two first-line options: antidepressant medications and psychotherapy. These are the established starting points, and they help a meaningful number of people, but they’re not the whole picture.
Treatment plans aren’t static. They change based on what a patient experiences: whether symptoms improve, whether side effects become a problem, and how the patient’s life and goals shift over time.
The National Institute of Mental Health notes that antidepressants typically take four to eight weeks to produce their full effect, and that some symptoms, like sleep and appetite, often improve before mood does. That’s a long runway for someone already in a depressive episode. It also means that what looks like a failed medication trial might just be one that needed more time, or it might genuinely not be working. Clinicians must hold that uncertainty and make a call.
What this means in practice is that a psychiatric treatment plan is less of a fixed protocol and more of an ongoing conversation between provider and patient.
Why Some Patients Need More Than First-Line Options
First-line treatments don’t land the same way for everyone. That’s a biological reality, not a reflection of how hard someone is trying.
The U.S. Department of Veterans Affairs states that approximately two-thirds of people diagnosed with depression do not get adequate relief from their first antidepressant trial. That’s a significant portion of patients. And it doesn’t account for the people who see some initial improvement but then plateau, or those who respond to medication but simply can’t tolerate the side effects well enough to stay on it.
The reasons first-line options fall short vary. Partial response is common. A patient might feel somewhat better, but not well enough to function the way they want. Side effects like weight gain, sexual dysfunction, or emotional blunting push others off medication before it has a fair chance. And some patients don’t respond at all despite trying multiple trials at adequate doses over adequate time.
When this pattern develops, clinicians start talking about treatment-resistant depression. It’s worth saying directly: Needing to move beyond initial depression treatment options is not a personal failure. It’s a recognized clinical reality. The brain doesn’t always respond to the same inputs the same way, and treatment plans are designed to account for that.
How Clinicians Decide the Next Step
Once it becomes clear that first-line options aren’t delivering enough, clinicians don’t simply pick the next item on a list. The process is more collaborative than that.
Providers review the patient’s full treatment history, including what was tried, for how long, at what dose, and what the outcome was. Symptom severity gets assessed. Functional impact matters, too: How is the person doing at work, in relationships, day to day? Patient goals factor in. Not every patient is looking for the same outcome, and that shapes which next step makes the most sense.
The VA/DoD Clinical Practice Guideline describes this approach as measurement-based care using structured assessments and symptom tracking to personalize decisions and make the patient an active partner in their own care. Treatment escalation is what a thoughtful treatment plan does when the current approach isn’t working.
This is also the point in the conversation where options like TMS therapy, ketamine treatment, Spravato, or other modalities might come up. There’s no “right” number of failed trials that automatically triggers a next step. Timing is individualized. What matters is whether the current approach is genuinely helping, and if not, what might.
Why TMS Therapy Is Often the Next Consideration
TMS therapy tends to come up at this stage for a few reasons, and those reasons have everything to do with how it works differently from what a patient has already tried.
TMS takes a more direct route than medication. Rather than working through the bloodstream, it applies magnetic pulses to a specific brain region, the left dorsolateral prefrontal cortex, which tends to show dampened activity in depression. It’s a completely different mechanism. For patients who haven’t responded to medication, that difference matters because it opens a pathway that oral antidepressants couldn’t reach.
The FDA clearance for the Ampa One TMS System explicitly positions TMS for adult patients with major depressive disorder who have not seen satisfactory improvement from prior antidepressant medication in the current episode. TMS is designed for exactly the situation many patients find themselves in after working through initial options without enough results.
There’s also growing clinical evidence supporting this sequence. A 2024 research published in the American Journal of Psychiatry found that in patients who hadn’t responded to two or more prior medications, rTMS was more effective at reducing depressive symptoms than switching to another antidepressant. That matters because it suggests that, after multiple medication trials, another medication switch may simply not be the strongest next option.
It’s also worth being clear about what TMS doesn’t replace. It isn’t positioned as a substitute for all other care. Most patients continue with therapy, and some continue with medication management alongside TMS. The goal isn’t to abandon what’s been working, even partially, but to add a new pathway when the existing ones have hit a ceiling.
A Thoughtful Progression, Not a Last Resort
Moving to TMS therapy is a strategic, evidence-based step in an evolving depression treatment plan. For many patients, it represents the moment when their care finally gets specific enough to address what standard approaches couldn’t.
Treatment-resistant depression is common. The data on first-line psychiatric treatment outcomes make that clear. What matters is that clinicians and patients keep working through the options rather than treating a partial response as good enough.
At Zeam, we work with patients through every stage of that process. Whether you’re just starting to explore TMS or you’ve already been through multiple medication trials without the relief you need, we’re here to help you understand what your options are and what the evidence says. If you’d like to talk through whether TMS therapy or another advanced approach might make sense for where you are right now, contact us to schedule a consultation.
Key Takeaways
- Depression treatment plans evolve over time – Clinicians adjust treatment based on patient response, side effects, and functional outcomes, making psychiatric care an ongoing, personalized process.¹
- First-line treatments don’t work for everyone – A significant portion of patients do not achieve adequate relief from their first antidepressant trial, leading to the need for additional options.²
- Treatment-resistant depression is common – Needing to move beyond initial treatments is a recognized clinical reality, not a failure, and often leads to consideration of advanced therapies.³
- TMS works through a different mechanism – Unlike medications that affect the whole body, TMS targets specific brain regions involved in mood regulation, offering a non-systemic alternative.⁵
- TMS is designed for patients who haven’t responded to medication – FDA-cleared TMS devices are specifically indicated for patients with major depressive disorder who have not improved with prior antidepressant treatment.⁴
- Research supports TMS after multiple medication trials – Clinical studies show that TMS can be more effective than switching antidepressants in patients who have not responded to previous treatments.⁵
- TMS is part of a broader treatment plan – Patients often continue therapy or medication alongside TMS, using it as an additional pathway rather than a replacement.³
- It’s a strategic step, not a last resort – TMS is introduced as part of a thoughtful, evidence-based progression in care, helping patients move forward when standard treatments reach their limits.³
Citations
- National Institute of Mental Health. Mental Health Medications.
https://www.nimh.nih.gov/health/topics/mental-health-medications - VA Community Care Clinical Determination for TMS
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00026.pdf - VA/DoD Clinical Practice Guideline for Major Depressive Disorder
https://www.healthquality.va.gov/guidelines/MH/mdd/VADoDMDDCPG_ProviderSummary_Final_508_updated.pdf - FDA Clearance Summary for TMS device (Ampa One System)
https://www.accessdata.fda.gov/cdrh_docs/pdf24/K243319.pdf - American Journal of Psychiatry study on rTMS effectiveness after medication failure
https://psychiatryonline.org/doi/full/10.1176/appi.ajp.20230556