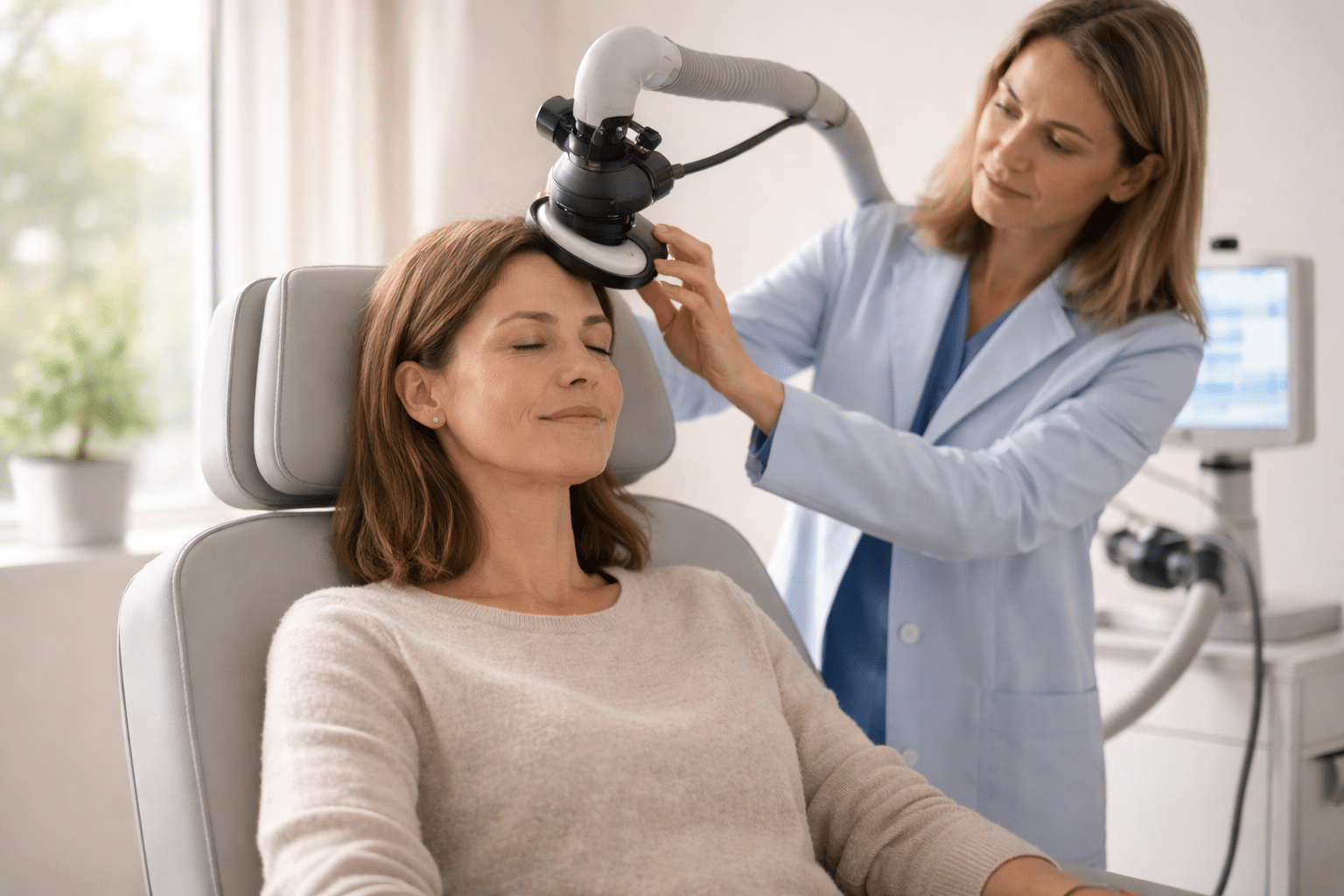
Deciding to move toward advanced depression treatment options can feel like standing at the edge of something unfamiliar. Transcranial magnetic stimulation, ketamine, and Spravato are some of the names that might sound clinical or a little intimidating. And if you have been living with depression for a while, the idea of stepping into something new brings up a lot. Hesitation is common here. Most people sit with it for weeks or even months before they feel ready to take another step.
This article is about why that pause happens, what fears or uncertainties show up, and how clinicians help patients think through it all without rushing.
Quick Answer Summary
Patients often delay moving to advanced depression treatments like TMS or ketamine due to fear of the unknown, past treatment fatigue, logistical concerns, and uncertainty about readiness. Research shows that lack of understanding, stigma, and prior unsuccessful treatments contribute to hesitation, while collaborative, patient-centered care helps individuals move forward at their own pace when they feel ready.
Key Takeaways
- Many patients delay advanced treatments due to fear and lack of familiarity with options like TMS or ketamine¹
- Treatment-resistant depression affects nearly 1 in 5 patients on medication, contributing to skepticism about new approaches²
- Practical barriers like time, cost, and insurance coverage can significantly impact decision-making¹
- Readiness is personal, and patients often need time to feel confident before moving forward
- Collaborative care models improve outcomes by respecting patient pace and addressing concerns directly¹
Fear of the Unknown
When most of your experience with mental health care involves a prescription bottle and a therapy appointment, anything outside that framework feels foreign. That is often the first layer of hesitation.
Advanced treatments like TMS or ketamine simply are not as familiar as a daily pill. Most people have never sat in a TMS chair. And they do not know what ketamine infusion therapy involves.
How does it feel while it is happening? Will it be uncomfortable? What if it does not work after all that effort? Those unknowns create a natural pause.
A 2024 national survey found that patients and caregivers often point to a “lack of understanding of the intervention” as a key reason they hold back from treatments like TMS and ECT. And for ketamine treatment, stigma still clings to the conversation. Some people worry about judgment from others or carry old, inaccurate ideas about what these therapies mean. It is hard to move forward when you are not even sure what forward looks like.
Past Treatment Fatigue and Hopelessness
If someone has tried two or three or four different medications and still feels stuck, that takes a toll. The energy required to hope and then feel disappointed again is real and heavy. That exhaustion often hardens into a quiet skepticism. The question that sits in the back of the mind is simple: “Why would this time be different?”
A 2025 study from the All of Us Research Program found that close to one in five (19.10%) people taking medication for depression actually meet the criteria for treatment-resistant depression. That means the usual approaches have not gotten the job done.
Living in that space wears down a person’s belief that anything can help. This is not stubbornness or pessimism. It is a completely understandable response to repeated letdowns.
Therefore, when a clinician suggests stepping up to something more intensive, the patient is not just weighing the treatment itself. They are also guarding against the possibility of yet another disappointment. That kind of fatigue needs someone who sees the exhaustion and does not try to rush past it.
Concerns About Time, Cost, and Logistics
Even when someone feels emotionally open to exploring advanced psychiatric treatment, the rest of life does not pause to accommodate it.
Take TMS, for example. The standard course involves daily sessions for four to six weeks. Ketamine or esketamine treatments require a driver and a period of monitoring in the office afterward. For someone managing a full-time job, young kids at home, or a long commute to the clinic, those logistics can feel impossible before the question of effectiveness even enters the picture.
Then there is the insurance piece. The same 2024 national survey mentioned earlier identified “lack of insurance coverage” as one of the most important barriers for TMS from the perspective of psychiatrists. Patients understandably do not want to get their hopes up only to find out their plan will not pay for the care they need.
Uncertainty About Whether They’re “Ready”
There is another kind of hesitation that is harder to put into words. It is the internal question of whether someone has truly earned the right to try something more advanced.
Patients sometimes worry that pursuing options like TMS or ketamine treatment means they are skipping steps. They might think they are not quite “sick enough” to justify it. The voice in the head says, “Maybe I should try just one more medication first,” or “Maybe I need to give therapy a little more time.” This is not resistance for the sake of resistance. It is a desire to feel certain before making a move that feels significant.
Patients do better when they are actively involved in treatment choices. But being involved also means sitting with doubt. Clinicians can help clarify when it makes clinical sense to move forward. Still, the internal timeline for readiness belongs to the patient. There is no universal clock ticking.
How Clinicians Help Patients Navigate These Delays
The good news is that a thoughtful clinician does not see hesitation as a problem that needs to be crushed. They see it as part of the conversation that needs to happen.
This is where a collaborative approach makes all the difference. A good clinician doesn’t push. They ask things like “What do you make of this so far?” or “What feels hardest to picture?” That kind of open invitation lets fears and misunderstandings surface so they can be addressed directly. Not brushed aside.
Sometimes the next step is not a full commitment to a course of ketamine infusion therapy or a month of daily TMS visits. It might be any of the following:
- A longer consultation
- A conversation with someone who has been through it already
- A plan to start small and see how it feels
Education happens without pressure. Respecting the patient’s pace is a core part of quality psychiatric treatment. It is not about convincing anyone but about walking alongside them while they figure out what comes next.
The Right Time Is Personal, Let’s Find It Together
Delaying advanced depression treatment options makes perfect sense once you look at everything that goes into the decision. Fear of what is unfamiliar, exhaustion from past attempts that did not work, real-world logistics like time and money, and that quiet inner question of whether you are ready all deserve attention, not impatience.
If you have been sitting with hesitation about options like TMS or ketamine treatment, we at Zeam are here to listen. Our team offers evidence-based psychiatric treatment, therapy, and advanced modalities all in one place. We believe the right pace is the one that feels like yours. Contact us today to have an honest conversation about what has been holding you back and whether it might be time to take the next step.
Citations
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11136602/
- https://www.sciencedirect.com/science/article/abs/pii/S016503272501300X?via%3Dihub