Starting TMS brings up a lot of questions. You might wonder if you’ll feel something right away. Or maybe you’re bracing yourself to feel nothing at all, because that’s just how these things seem to go sometimes. That mix of hope and hesitation is standard for anyone stepping into a new kind of psychiatric treatment.
The truth is that early responses to TMS are all over the map. Some people catch small changes in the first week or two. Others need more time before anything shifts.
This blog walks through what those early weeks look like, explains how your care team tracks things behind the scenes, and shows where TMS fits into a bigger plan.
Quick Answer Summary
In the early stages of TMS therapy, most patients experience mild physical sensations like tapping on the scalp and occasional headaches, while emotional improvements tend to be subtle or delayed. Some people notice small changes in sleep, energy, or thought patterns within the first two weeks, but many feel no immediate difference. Clinicians track progress using tools like the PHQ-9, and meaningful results typically emerge after several weeks of consistent treatment.
Key Takeaways
- Early TMS sessions often involve mild scalp sensations and temporary discomfort as the brain adjusts¹
- Emotional improvements in the first 1–2 weeks are usually subtle or not immediately noticeable²
- Tools like the PHQ-9 help clinicians track small but meaningful progress over time¹
- Lack of early results does not indicate treatment failure, as changes build gradually²
- TMS is most effective as part of a broader treatment plan including therapy or medication²
- Most significant improvements occur after completing a full 4–6 week treatment course²
The First Few Sessions
The first day is about getting the settings dialed in. You’re awake, you’re in a chair, and there’s no downtime needed once it’s over.
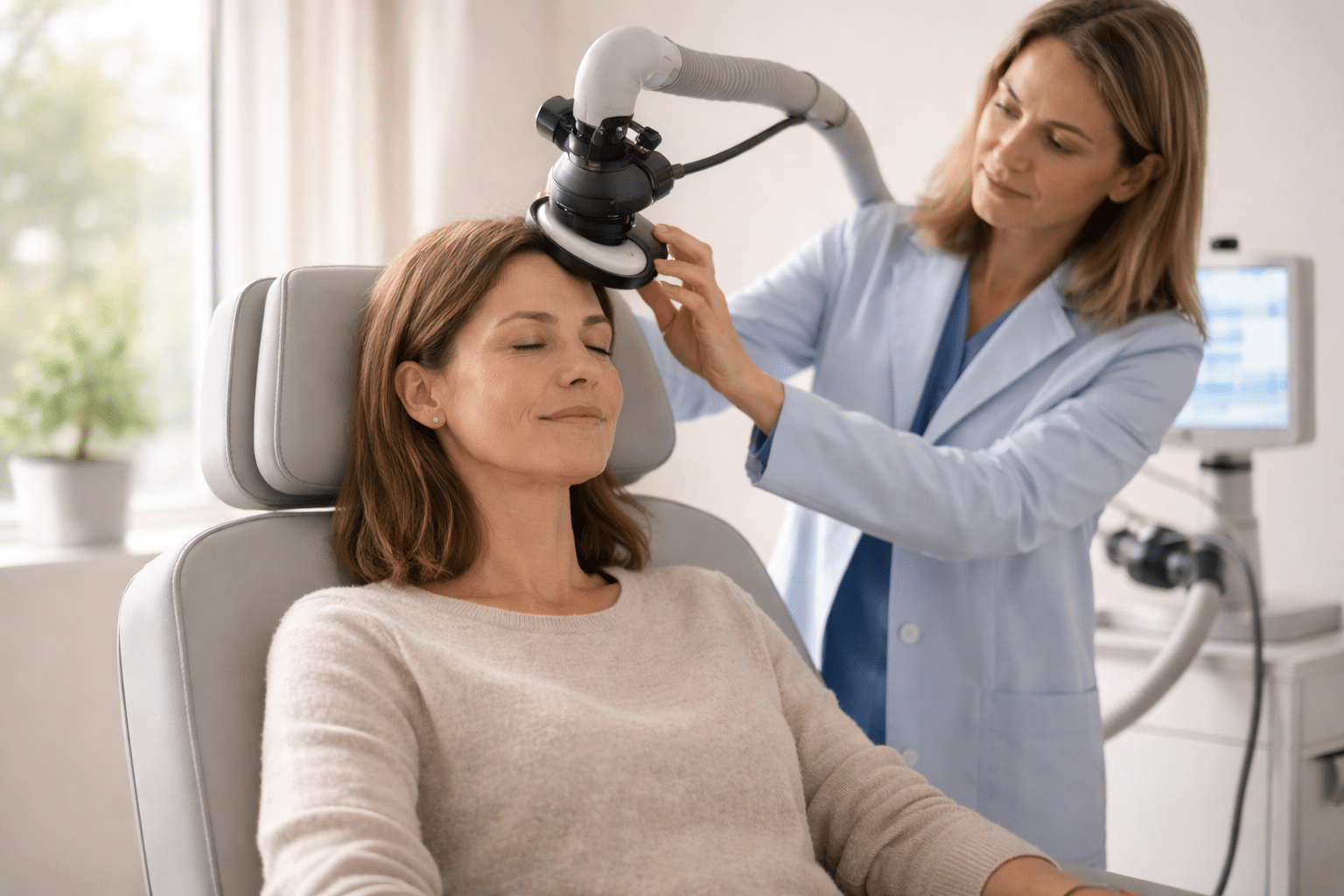
You’ll sit reclined while a coil rests against a specific spot on your head. The sensation people talk about most is a tapping or knocking feeling on the scalp, timed with a clicking sound. It’s weird for a minute. But then your brain kind of accepts it and moves on. The person running the machine starts things off at a lower intensity and inches it up to where it needs to be. They’ll check in to make sure you’re still comfortable.
Some people get a mild headache or a little tenderness where the coil sits. That’s common in the first few days. It tends to ease up as your scalp gets used to the sensation. When the session wraps up, which takes about twenty minutes, you’re free. You can drive, go back to work, and grab coffee.
Early Changes Patients May Notice
Some patients notice subtle things in those first two weeks of depression treatment. It’s rarely a dramatic moment where the clouds part.
It’s smaller. Maybe you sleep through the night without waking up at three in the morning with your mind spinning. Maybe you find the energy to load the dishwasher without it feeling like a whole production. Some people say their thoughts feel a tiny bit less sticky, like the negative loop isn’t gripping quite as hard.
Then there are many people who feel nothing. No change at all. Not yet.
If you’re in that second group, it’s not a sign that the treatment is failing. The brain pathways that TMS is nudging have been stuck in a rut for a long time. It takes repeated sessions to coax them out. Not noticing a shift in week one or two is a totally normal part of the process.
How Clinicians Monitor Progress During Early TMS
You might not notice the tiny changes happening day by day. That’s where your care team steps in with tools that are more sensitive than our own internal radar. This kind of tracking is just part of good psychiatric treatment.
At the start and then at regular checkpoints, you’ll likely fill out the PHQ-9, a short list of questions about sleep, appetite, mood, and interest in things. This little questionnaire is good at catching the specific kind of improvements that come with TMS. Even if your total score looks flat week after week, your clinician is looking at which boxes are shifting. Maybe you’re still tired, but the “feeling hopeless” box is a little less checked than before. That’s a data point.
That data helps steer the ship. If after a chunk of sessions, there’s absolutely zero movement on paper, your provider might think about tweaking the placement or the intensity. On the flip side, seeing those tiny paper gains can be reassuring. It’s proof that something is stirring underneath, even if you haven’t consciously felt a good day yet.
How TMS Fits Within a Broader Psychiatric Treatment Plan
TMS is rarely the only player on the field. It slots into a bigger, coordinated strategy.
For a lot of people, that means sticking with their regular medication while doing TMS. The two can work side by side. It also usually means keeping up with a therapist. TMS is working on the wiring, but therapy is working on the thinking habits that grew up around the depression.
Some patients, depending on their history and how things are going, might also consider other interventional options down the line. That could mean looking into ketamine therapy, which works on a different chemical system and tends to move faster, though it’s a different kind of process with different monitoring needs.
The main idea is that TMS is one piece of a puzzle your psychiatrist is putting together and adjusting based on how you’re doing, week by week.
Setting Realistic Expectations for the Early Phase
The early part of TMS is like laying down a foundation. You don’t see the house yet, but the ground is getting ready. The real visible changes usually come with the full course of depression treatment.
A standard course is daily sessions for about four to six weeks. That’s the window where most people see the real movement. A big review that looked at over 5,000 real-world patients found response rates between 58% and 83% and remission rates between 28% and 62%. Those are solid numbers, but they’re snapshots taken at the finish line, not at the starting block.
If you’re in week one or two, the best thing you can do is keep showing up and try not to overthink every little sensation or non-sensation. The work is happening at a level you can’t feel. Patience is built into the treatment design.
Let Zeam Guide Your Journey
The early weeks of TMS come with some physical adjustments, some quiet monitoring, and a lot of waiting. For some people, that waiting brings little hints of relief, like a decent night’s sleep, a slightly quieter mind. For others, it’s just the hum of the machine and a hope that something’s happening underneath. Both experiences are part of the normal range for this kind of psychiatric treatment.
Here at Zeam, we track that whole journey alongside you. We use the data from your sessions and your own words to make sure TMS fits right into your complete care plan, whether that’s alongside medication, therapy, or maybe other paths like ketamine therapy if needed. If you’re thinking about TMS, our team will watch your progress closely and make sure it lines up with your overall depression treatment goals. Contact us today to schedule a consultation and start with clarity and support.
Citations
- Patient Health Questionnaire (PHQ-9) Overview
https://www.apa.org/depression-guideline/patient-health-questionnaire.pdf - Clinical Outcomes and Effectiveness of TMS Therapy
https://www.sciencedirect.com/science/article/pii/S1388245724003766