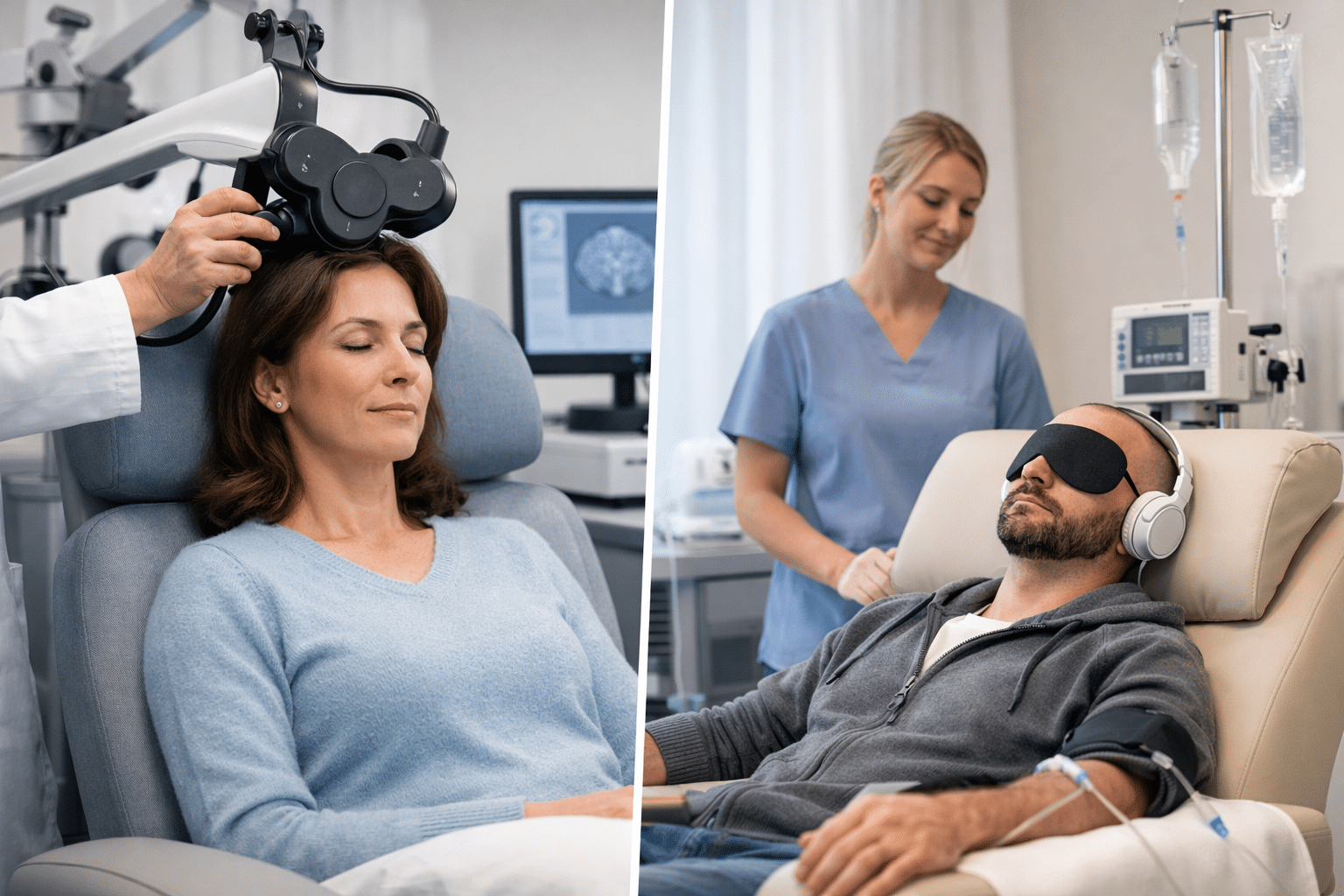
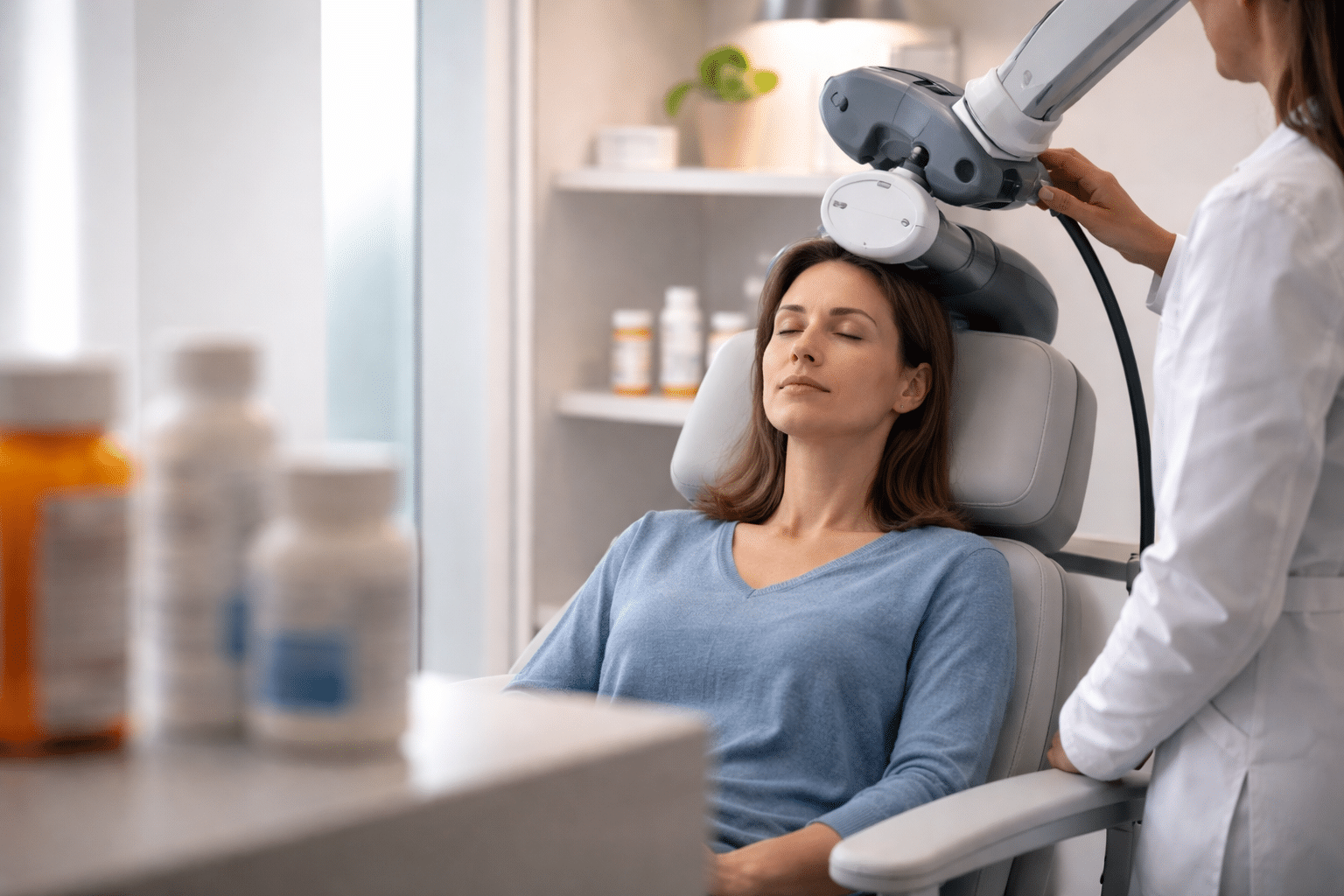
When first-line depression treatment hasn’t provided enough relief, the next step isn’t obvious. There’s no universal protocol that automatically points every patient toward one specific option. The path forward is personal, built from clinical data, lived experience, and a lot of careful conversation between patient and provider.
This article walks through the key factors clinicians consider when recommending advanced options. If you’re trying to understand how these decisions get made, or why two people with the same diagnosis might end up on different paths, this should help.
Quick Answer Summary
Clinicians recommend advanced depression treatments like TMS or ketamine based on multiple factors, including treatment history, symptom severity, urgency, medical safety, lifestyle constraints, and patient preferences. There is no one-size-fits-all approach. Instead, providers use shared decision-making and individualized evaluation to determine the most appropriate path forward for treatment-resistant depression.
Patient History and Previous Treatment
The first thing a clinician does is look back before looking forward. A thorough review of what has and hasn’t worked forms the foundation of any advanced psychiatric treatment recommendation.
That means asking specific questions:
- How many antidepressant trials has this person completed?
- What types of therapy have they tried, and for how long?
- How long has the current episode lasted?
The National Institute of Mental Health notes that antidepressants typically take four to eight weeks to produce meaningful results, which means a provider also needs to assess whether past trials were long enough to count as fair tests.
This matters enormously because history shapes everything that follows. According to a clinical determination from the VA, roughly two-thirds of people with depression don’t get adequate relief from their first antidepressant.
That gap between what medication promises and what it delivers is one of the main reasons advanced options enter the conversation at all. A detailed treatment history helps clinicians determine whether a patient meets the criteria for treatment-resistant depression and, crucially, which mechanisms haven’t been tried yet.
Symptom Profile and Urgency
Not all depression looks the same, and the specific pattern of symptoms can push a recommendation in a particular direction.
Urgency
Speed of relief is sometimes the most pressing clinical concern. The NIMH highlighted in a 2024 science update that while most antidepressants take weeks or even months to work, ketamine can begin reducing depression symptoms within hours in some patients who haven’t responded to other treatments. When there’s acute suicidal ideation or severe functional impairment, when waiting another month for a medication trial to run its course isn’t a realistic option, that speed difference becomes a genuine clinical factor.
Symptom Pattern
Beyond urgency, the nature of the symptoms themselves matters. Someone whose depression is characterized primarily by low energy, withdrawal, and difficulty concentrating may be a strong candidate for TMS, which targets specific brain regions associated with mood regulation.
The FDA’s clearance of the Ampa One TMS system covers adults with major depressive disorder who haven’t seen satisfactory improvement from prior antidepressant medication. The device targets areas like the left dorsolateral prefrontal cortex, where activity is often reduced in depression.
Co-Occurring Conditions
Anxiety, PTSD, and chronic pain don’t stay neatly separate from depression. When they’re present, they can shift which advanced option makes the most sense, either because one treatment addresses overlapping symptoms or because certain options carry risks that interact with those conditions.
Medical Considerations and Safety
Safety always comes first, and medical factors can either open or close the door on certain options. This is where the clinical conversation gets highly individualized.
TMS isn’t right for everyone. Metal implants in or near the head can interfere with the magnetic field, which rules it out for some patients immediately.
Ketamine treatment, including esketamine (Spravato), brings a different set of considerations. The FDA’s prescribing information for Spravato requires at least two hours of post-session monitoring because of sedation, dissociation, and respiratory risks. Clinicians also look at blood pressure, as uncontrolled hypertension is a real concern before any ketamine-based option gets recommended.
Medication interactions also come into play. A person’s current psychiatric medications, cardiovascular health, and overall medical stability all factor into which advanced option can be offered safely. This is a nuanced clinical assessment that takes the whole person into account.
Logistics and Commitment
Even when the clinical case for a particular treatment is strong, real-world factors matter. A clinician who doesn’t account for them is setting a patient up to struggle with follow-through.
Schedule
TMS typically involves daily sessions over four to six weeks, up to 36 sessions according to VA clinical guidelines. Ketamine therapy, depending on the format, follows a different rhythm: infusions delivered in a series, or esketamine administered twice weekly in the first month, then tapering based on response. Neither schedule is objectively “easier,” but one may fit a patient’s work schedule, childcare situation, or energy levels better than the other.
Transportation
This one catches people off guard. Ketamine requires a driver after every session. That’s not a minor logistical footnote. For someone without reliable transportation support, it can be a real barrier to consistent treatment.
Insurance Coverage and Access
Coverage for advanced options varies significantly. Some patients have robust insurance support for TMS; others don’t. Clinicians help patients think through what’s accessible given their coverage, and sometimes that shapes the recommendation more than anyone would prefer.
Patient Preference and Values
This might be the factor that gets the least attention in clinical literature, but it’s central to how good recommendations get made. Shared decision-making and measurement-based care are the standard when depression treatment becomes more complex. Once the clinical picture is clear, what the patient wants has to be part of the equation.
Some patients want to avoid additional medications and are drawn to TMS as a non-drug option. Others are open to ketamine treatment but have concerns about the dissociative experience and need honest information before they can commit. Some patients have read a lot and arrive with strong preferences; others want to be guided more directly. None of these is wrong. Shared decision-making ensures that the recommendation accounts for what matters most to the individual patient, not just what the data suggests is the most effective option in aggregate.
A Roadmap Built for You
Advanced depression treatment recommendations are built from a lot of moving parts: your treatment history, the specific shape of your symptoms, your medical background, the practical realities of your schedule and support system, and your own values and preferences. No single factor determines the outcome, and the goal isn’t to find the most common answer but to find the right answer for you. That kind of individualized care is the standard that quality psychiatric treatment aspires to.
At Zeam, we take all these factors seriously. Our team in Sacramento, Folsom, and Roseville works through the full picture with each patient before recommending an advanced path forward, whether that’s TMS, one of our ketamine treatment options, or something else entirely. Ready to talk through your options? Contact us today to schedule a consultation.
Key Takeaways
- Treatment history shapes next steps – Clinicians review past antidepressant trials and therapy experiences to determine whether a patient meets criteria for treatment-resistant depression and which options have not yet been explored.¹
- Symptom urgency influences treatment choice – When rapid relief is needed, such as in cases of acute distress or suicidal ideation, fast-acting treatments like ketamine may be prioritized.³
- Symptom patterns guide recommendations – Different depression profiles, such as low energy or withdrawal, may align better with targeted treatments like TMS that focus on specific brain regions.²
- Medical safety determines eligibility – Certain conditions, such as metal implants for TMS or cardiovascular risks for ketamine, can limit which treatments are safe for a patient.⁴
- Logistics play a major role – Treatment schedules, transportation requirements, and time commitments can influence whether a patient can realistically follow through with a specific therapy.²
- Insurance and access affect decisions – Coverage for advanced treatments varies, and accessibility can shape which options are available to a patient.²
- Patient preferences matter – Shared decision-making ensures that treatment plans align with a patient’s comfort level, goals, and values, not just clinical data.¹
- Personalized care leads to better outcomes – Advanced depression treatment is most effective when it is tailored to the individual, integrating clinical evidence with real-world factors and patient input.¹
Citations
- National Institute of Mental Health. Mental Health Medications.
https://www.nimh.nih.gov/health/topics/mental-health-medications - VA Community Care Clinical Determination for TMS
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00026.pdf - National Institute of Mental Health. New Hope for Rapid-Acting Depression Treatment.
https://www.nimh.nih.gov/news/science-updates/2024/new-hope-for-rapid-acting-depression-treatment - VA Community Care Clinical Determination for Ketamine / Esketamine
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00030.pdf