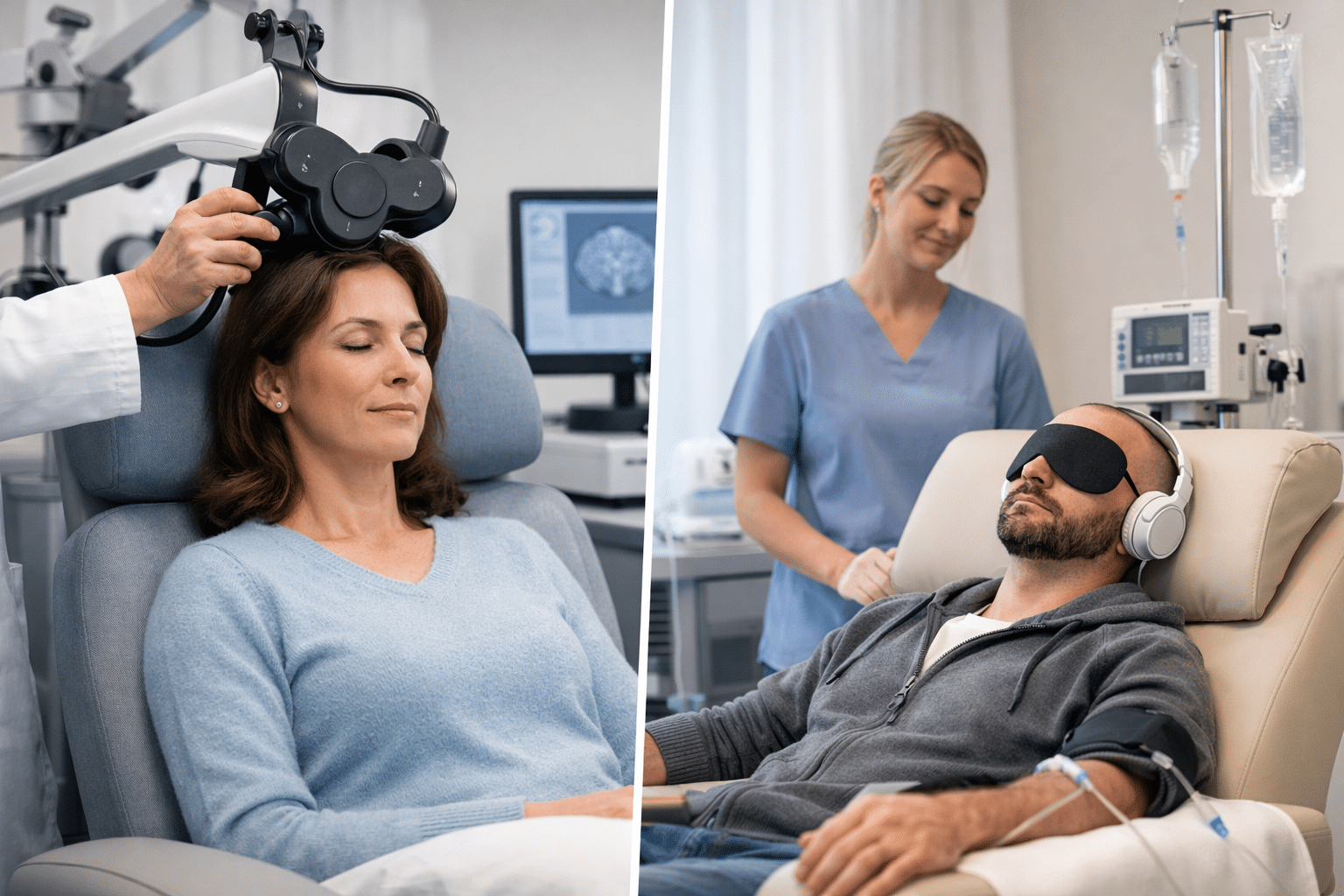
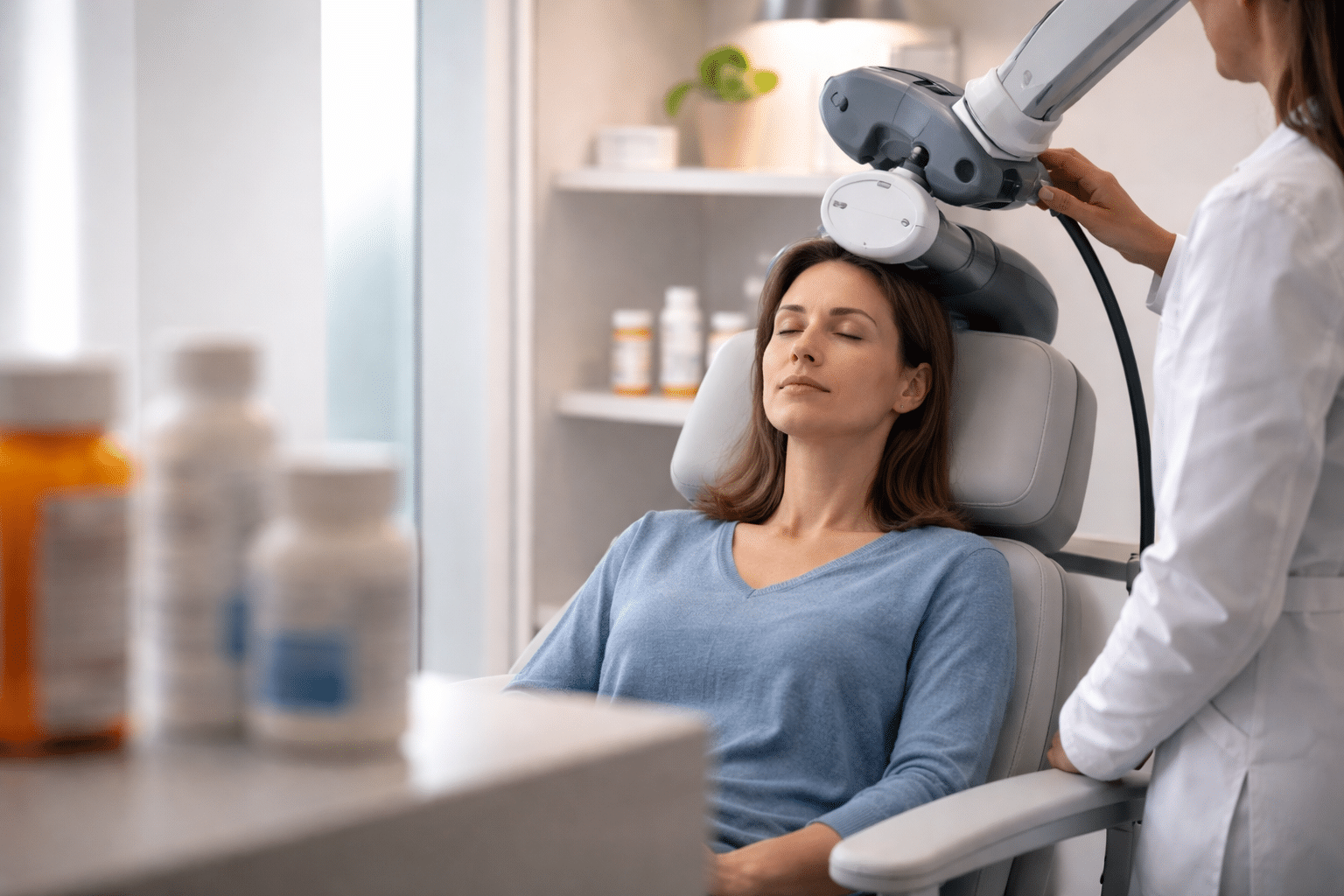
When standard depression treatment options haven’t worked, patients are often told there are still other paths forward. Two of the most talked-about are TMS therapy and ketamine therapy. Both have real evidence behind them. Both are offered in clinical settings for people who haven’t gotten enough relief from medications alone. But they are not the same thing, and clinicians don’t treat them as interchangeable.
The decision between them is shaped by a patient’s history, how quickly they need relief, what their body can tolerate, and what their daily life allows. This article walks through how that thinking tends to work inside a broader psychiatric treatment plan.
Quick Answer Summary
Clinicians choose between TMS therapy and ketamine therapy based on factors such as symptom urgency, treatment history, medical considerations, and patient preferences. Ketamine therapy may be preferred when rapid symptom relief is needed, as it can act within hours, while TMS therapy is often selected for patients seeking a non-medication, gradual approach with fewer systemic side effects. Both treatments are evidence-based options for treatment-resistant depression and are typically integrated into a broader psychiatric care plan.
Understanding the Two Options at a Glance
TMS Therapy
Transcranial magnetic stimulation is a noninvasive procedure. A clinician places an electromagnetic coil against the scalp, and it delivers magnetic pulses that target areas of the brain showing reduced activity in people with depression.
Repetitive TMS (rTMS) is typically used for moderate to severe depression when medications have been ineffective or intolerable. Sessions run 3 to 40 minutes, usually five days a week for four to six weeks. No anesthesia, sedation, or recovery time after each visit.
Ketamine Therapy
Ketamine treatment works differently and through an entirely different part of the brain. Ketamine bypasses the serotonin and dopamine pathways entirely, targeting glutamate instead, a mechanism linked to neuroplasticity and faster symptom relief. It’s administered in a supervised clinical setting, either as an IV infusion or as intranasal esketamine (the FDA-approved form, Spravato). Patients are monitored for at least two hours after each session and given risks like sedation and dissociation.
Both TMS and ketamine treatments are evidence-based options for treatment-resistant depression, and both are placed later in the care pathway, not at the starting line.
Key Factors That Guide the Decision
According to the VA/DoD Clinical Practice Guideline, when depression becomes harder to treat, there is no universal formula for choosing between options like TMS, ketamine, or esketamine. The guideline emphasizes shared decision-making because the evidence doesn’t support one single answer for every patient.
Here are the main factors clinicians typically weigh.
Symptom Profile
How urgent is the need for relief? That question matters a lot. Unlike standard antidepressants, ketamine can begin reducing depressive symptoms within hours for some patients, not weeks. That speed difference is clinically significant. If a patient is in acute distress or experiencing suicidal ideation, that timeline changes what’s being considered.
TMS, by contrast, builds results more gradually. Some newer accelerated protocols can shorten the course, but traditional TMS is still a steady, multi-week process. If slower improvement is acceptable and the patient’s situation is stable, that may be a reasonable fit.
Treatment History
The VA’s Community Care Clinical Determination for TMS notes that about two-thirds of patients with depression don’t get adequate relief from their first antidepressant trial. That’s a large group.
What those patients tried, how they responded, and which side effects became barriers all factor into what a clinician recommends next. Someone who has tried multiple medication classes without success may be a stronger candidate for a different mechanism of action, which is where both TMS and ketamine treatment enter the picture.
Medical Considerations
Some patients aren’t candidates for one approach regardless of preference. TMS has contraindications related to metallic implants near the head. Ketamine-based treatment carries cardiovascular monitoring considerations and requires post-session observation time. A patient’s full medical picture shapes what’s on the table.
Patient Preference
Daily TMS visits over four to six weeks suit some patients well. Others find that schedule harder to maintain. Ketamine treatment runs fewer sessions overall, but each one requires post-session monitoring, and IV infusions tend to stretch into a longer maintenance rhythm.
The Pfeiffer et al. study tracked veterans averaging 18 infusions across 12 months, starting at roughly every five days before gradually spacing out. Both paths ask something real of the patient. The commitment just looks different.
When TMS Therapy May Be the Preferred Choice
For some patients, the appeal of TMS starts with what it isn’t. No medication means no new side effects to manage, and for someone who has spent years navigating weight gain, disrupted sleep, or sexual dysfunction from antidepressants, that matters more than it might sound.
The daily schedule is a real ask, but it works for patients whose lives can accommodate it. It also tends to fit better when the clinical picture isn’t urgent, when depression treatment looks more like persistent low energy and withdrawal than acute crisis. And because there’s no sedation or dissociation involved, patients walk out of each session the same way they walked in. That kind of normalcy isn’t minor.
When Ketamine Therapy May Be the Preferred Choice
Ketamine therapy becomes more relevant when the clinical picture involves urgency. Acute suicidal ideation is one scenario where its rapid-acting properties have real value. Beyond that, patients who have worked through multiple medication classes across different antidepressant types and still haven’t responded may benefit from a mechanism that operates outside the monoamine pathway entirely.
There’s also a practical reality: Some patients prefer a shorter series of supervised sessions over daily office visits. The Pfeiffer et al. study found that 26% of veterans achieved clinical response and 15% reached remission by six weeks of IV ketamine treatment. These results came through routine care, not a controlled trial setting. That’s a meaningful signal for clinicians weighing options.
A Personalized Path Forward
Choosing between TMS and ketamine therapy isn’t really about which one is better in the abstract. It’s about which one fits this particular person: their history, their symptoms, their urgency, and what they can realistically sustain.
The VA/DoD guideline is honest that the research still doesn’t offer a clean head-to-head answer. What it does support is the value of individualized, measurement-based decision-making over rigid algorithms. Both options are legitimate, evidence-backed tools in modern psychiatric treatment. Neither is a last resort, and neither is a guarantee.
At Zeam, we take exactly this kind of approach. Our team in Sacramento, Folsom, and Roseville evaluates each patient’s full picture before recommending TMS, ketamine, or any combination of services, and we don’t separate the clinical decision from the person making it. If you’re exploring advanced options for treatment-resistant depression, we’re here to help you work through the choice. Contact us today to schedule a consultation and take the next step toward relief.
Key Takeaways
- Both TMS and ketamine are used for treatment-resistant depression – These therapies are typically considered after patients have not responded adequately to standard antidepressant treatments.¹
- There is no one-size-fits-all answer – Clinical guidelines emphasize shared decision-making, as evidence does not support a single “best” option for every patient.¹
- Ketamine offers faster symptom relief – Ketamine therapy can begin reducing depressive symptoms within hours for some patients, making it especially relevant in urgent situations.³
- TMS provides a non-medication alternative – TMS therapy does not involve systemic medication and is often preferred by patients who cannot tolerate antidepressant side effects.²
- Treatment timelines and commitments differ – TMS typically requires daily sessions over several weeks, while ketamine involves fewer sessions but longer appointments with post-treatment monitoring.³
- Medical factors can limit options – Certain conditions, such as metallic implants for TMS or cardiovascular concerns for ketamine, may influence which treatment is appropriate.²
- Patient lifestyle and preference matter – The choice between TMS and ketamine often depends on what a patient can realistically commit to, including scheduling, monitoring requirements, and comfort with each approach.¹
- Personalized care leads to better outcomes – Clinicians rely on individualized evaluation and ongoing monitoring rather than rigid protocols to determine the best treatment path.¹
Citations
- VA/DoD Clinical Practice Guideline for Major Depressive Disorder
https://www.healthquality.va.gov/guidelines/MH/mdd/VADODMDDCPGFinal508.pdf - VA Community Care Clinical Determination for TMS
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00026.pdf - Pfeiffer et al., clinical outcomes of IV ketamine in veterans
https://pubmed.ncbi.nlm.nih.gov/38206011/