If you’ve tried antidepressants and nothing has stuck, you know how exhausting that process gets. The adjustments, the waiting, the side effects, and then starting over with something new.
For people dealing with treatment-resistant depression, that cycle can go on for years. Standard depression treatment options tend to work through the same basic pathway, which is why some people respond, and others don’t.
Ketamine infusion therapy takes a different approach entirely, one that’s drawn serious clinical attention over the past decade for how quickly it can act and where it works in the brain.
This article breaks down what the therapy involves, how sessions are structured, and what clinicians look for when tracking progress.
Quick Answer Summary
Ketamine infusion therapy is an intravenous treatment used for depression, particularly in treatment-resistant cases. Unlike traditional antidepressants that target serotonin, ketamine works through the brain’s glutamate system, promoting neuroplasticity and potentially delivering rapid symptom relief. Treatment typically involves a series of monitored infusions in a clinical setting, where clinicians track progress using symptom scales and patient feedback. Its structured protocol and different mechanism make it a valuable option within modern psychiatric care.
What Is Ketamine Infusion Therapy?
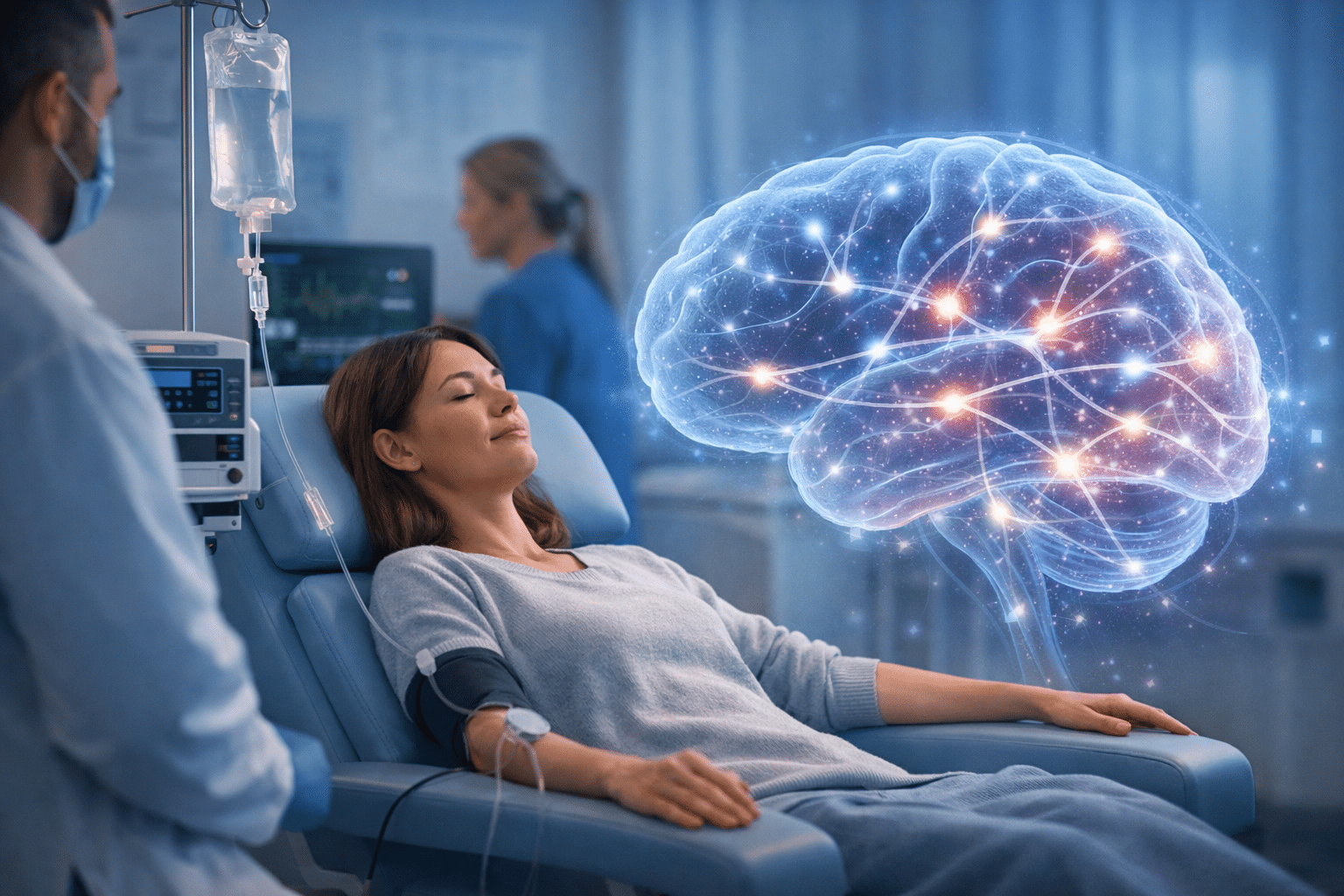
Ketamine infusion therapy is the intravenous administration of low-dose ketamine in a supervised clinical setting. Ketamine has been FDA-approved as an anesthetic since the 1970s.
Its use in psychiatry came later, and the IV form is still considered off-label for depression, used based on clinical evidence rather than a formal FDA psychiatric approval. The nasal spray version, esketamine, has FDA approval for treatment-resistant depression. IV ketamine does not. Even so, IV ketamine has a substantial research base and remains widely used in specialized clinical settings.
As a controlled medication in a clinical setting, this is a far cry from illicit use. Dosing is precise, the environment is monitored, and the protocol is built specifically to produce antidepressant effects.
How Ketamine Works Differently
Most antidepressants, such as SSRIs, SNRIs, and tricyclics, target serotonin or norepinephrine. They’re effective for many people, but they’re slow. Ketamine doesn’t work on those same systems.
Antos et al. describe NMDA receptor blockade, glutamate signaling, and downstream plasticity pathways as leading explanations for ketamine’s rapid antidepressant effects. The biology is still being worked out, but the mechanism looks different from standard serotonin-based antidepressants.
A registered systematic review by Kang et al. highlighted molecules such as BDNF, mTOR, and AMPA receptors as part of the neuroplasticity model linked to ketamine’s rapid antidepressant effects. Some patients notice a shift within hours or days, not weeks. That speed is one reason ketamine has drawn so much clinical attention in treatment-resistant depression.
The Treatment Setting
The clinical environment matters more in ketamine treatment than in most outpatient psychiatry, both because patients are monitored throughout and because comfort during the session can affect how people respond.
Infusions take place in a quiet, private room with vitals monitoring equipment and a trained clinician or nurse present at all times. Most programs prioritize the setting: a reclining chair, low lighting, and sometimes soft music.
Patients remain awake and aware throughout; there’s no general sedation. Some people describe the experience as deeply calming, while others notice mild perceptual shifts. Staff are present throughout to address any discomfort.
A Typical Infusion Session
Preparation
Before the medication starts, the team checks vital signs and places an IV line, usually in the arm. Most clinics do a brief pre-session check-in to gauge how you’ve been since the last visit. Then you settle in.
The Infusion
The standard protocol delivers ketamine at a subanesthetic dose, approximately 0.5 mg/kg, intravenously over about 40 minutes. Research by Shiroma et al. used this delivery window across both single and repeated infusion protocols.
Vital signs are monitored continuously. The dose is low enough that most people remain alert, though mild dissociative sensations, a sense of detachment from surroundings, are common and expected.
The Experience
Patients most commonly describe relaxation, a floaty or detached feeling, and sometimes an altered perception of time or space. These effects are temporary, typically fading within 30 to 45 minutes after the infusion ends. For many people, it’s the first time something has interrupted the pull of depressive thinking, even briefly.
Recovery
After the infusion, you stay for observation until your vitals stabilize. Because ketamine can impair attention and judgment after treatment, clinics usually require patients to arrange a ride home and avoid driving until the effects have fully worn off.
Some people notice mood changes the same day. Others feel the shift more gradually over the following 48 to 72 hours.
The Initial Series
A single infusion can produce measurable results, but most programs are built around a series. The typical protocol is six infusions over approximately two to three weeks.
The rationale is the cumulative effect. In the open-label Bio-K study, 52% of 74 participants with treatment-resistant depression reached remission after three infusions over 11 days. That result is encouraging, though the study was not blinded.
A five-year longitudinal study in Psychiatry Research tracked 71 real-world outpatients with treatment-resistant depression and found that roughly 55% responded to IV low-dose ketamine treatment, with side effects transient and mild in the large majority.
Not everyone responds at the same pace. Some notice a shift after the first or second infusion, others not until the full series is complete.
How Clinicians Monitor Your Progress
Every session comes with a check-in. Before the medication starts, your care team wants to know how the last few days went regarding sleep, mood, and any changes worth noting.
Most programs also use standardized scales, like the PHQ-9 or the Montgomery-Åsberg Depression Rating Scale (MADRS), to track symptom changes across the series. The MADRS specifically has been a primary outcome measure in ketamine treatment clinical trials, including the translational psychiatry RCT by Shiroma et al., comparing single versus repeated infusions. Numbers give clinicians something concrete to act on, not just a general sense of whether things are better or worse.
Dosing, session frequency, and what comes next all get shaped by this ongoing picture. Ketamine therapy for depression works best when the program stays responsive.
A New Path Forward
Ketamine infusion therapy has become one of the more significant developments in depression care in recent years, not because it works for everyone, but because it works through a fundamentally different mechanism than what most people with treatment-resistant depression have already tried. The delivery protocol is structured and clinically supervised, progress is tracked closely, and the evidence base is substantial.
It’s a monitored medical procedure with a clear clinical rationale and individualized oversight. For people who have exhausted other options, that structure matters as much as the science.
At Zeam in Sacramento, Folsom, and Roseville, we’ve built our ketamine therapy for depression program around that same philosophy. Comprehensive care, personalized from the start, integrated with everything else we offer in psychiatry and therapy. If other depression treatment options have left you back at square one, we’d like to talk. Reach out today to schedule a consultation.
Key Takeaways
- Ketamine infusion therapy is a clinically supervised treatment – It involves low-dose intravenous ketamine administered in a controlled medical setting with continuous monitoring to ensure safety and effectiveness.
- It works through a different brain pathway – Unlike traditional antidepressants, ketamine targets the glutamate system, influencing neural plasticity and potentially enabling faster symptom relief.¹
- Effects can occur rapidly – Some patients experience improvements within hours or days, rather than the weeks typically required for SSRIs or SNRIs.²
- Treatment follows a structured protocol – A typical course includes six infusions over two to three weeks, allowing cumulative effects to build over time.⁵
- The experience is controlled and monitored – Patients remain awake during infusions, with clinicians tracking vital signs and ensuring comfort throughout the session.
- Neuroplasticity plays a key role – Research highlights mechanisms involving BDNF, mTOR, and AMPA receptors, which are associated with synaptic repair and mood improvement.¹
- Progress is measured throughout treatment – Clinicians use standardized tools like PHQ-9 and MADRS, along with patient feedback, to adjust dosing and treatment plans.
- It’s designed for treatment-resistant depression – Ketamine is typically considered after multiple antidepressant trials have failed to produce sufficient improvement.
Citations
- MDPI. Molecular Mechanisms of Ketamine in Depression Treatment.
https://www.mdpi.com/1422-0067/25/24/13658 - Frontiers in Psychiatry. Ketamine’s Rapid Antidepressant Effects.
https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2022.860882/full - Nature Translational Psychiatry. Ketamine infusion clinical trial outcomes.
https://www.nature.com/articles/s41398-020-00897-0 - Michigan Medicine. Ketamine’s promise and ongoing research questions.
http://www.michiganmedicine.org/health-lab/ketamines-promise-severe-depression-grows-major-questions-remain - Psychiatry Research. Long-term outcomes and response rates in IV ketamine therapy.
https://www.sciencedirect.com/science/article/pii/S0165178124001501