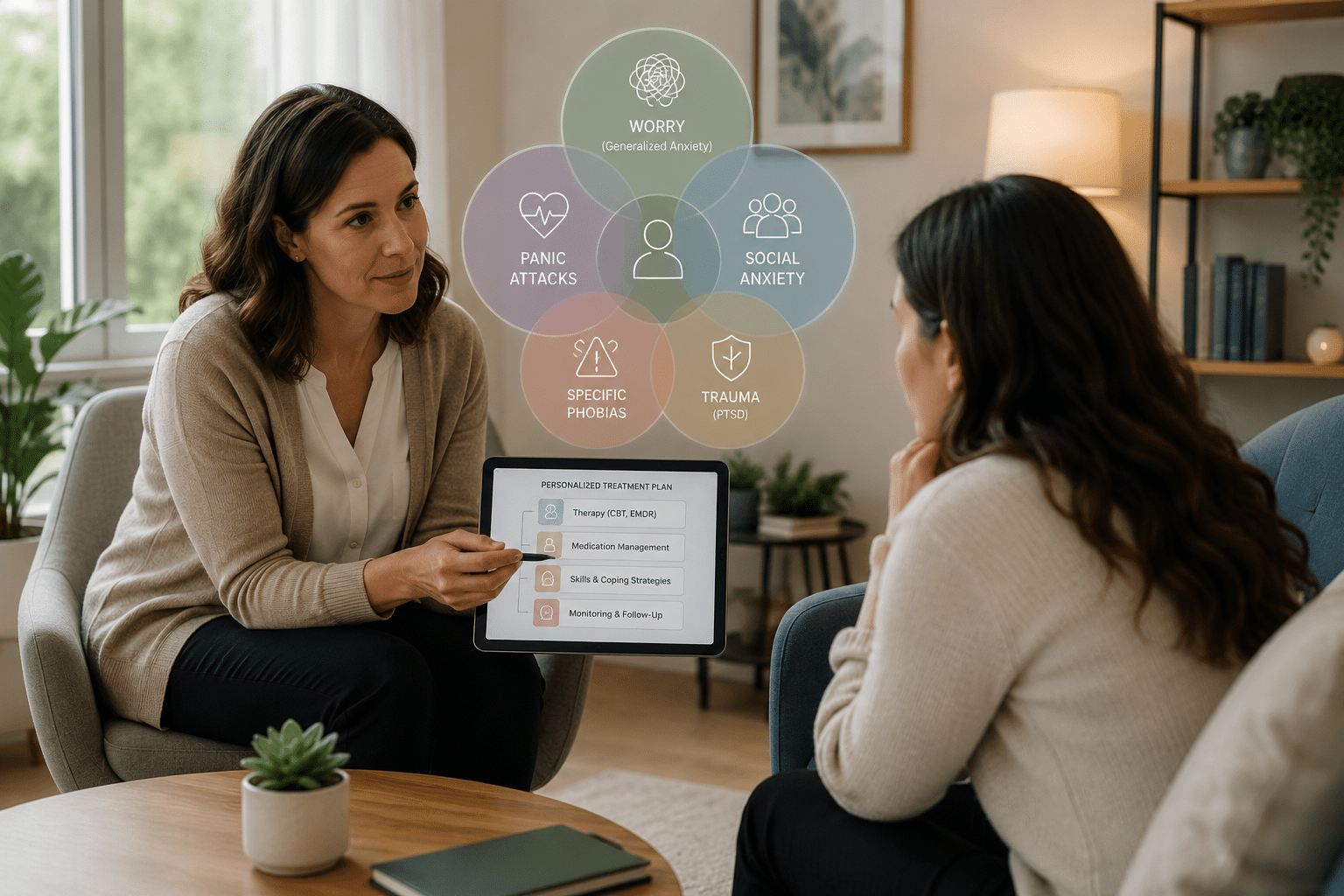
Most people who seek help for anxiety don’t walk in with one clean diagnosis. It’s common to have generalized anxiety running alongside panic attacks, social avoidance, specific phobias, or PTSD symptoms, sometimes all at once.
Research shows that 60% of people diagnosed with one anxiety disorder have at least one additional anxiety or depressive diagnosis. That overlap is the rule, not the exception.
This article explains how clinicians structure care when the picture is that complicated, how therapy and psychiatric treatment get coordinated, why treatment is built in layers, and what patients can realistically expect from that kind of approach.
Quick Answer Summary
Clinicians treat multiple anxiety disorders using a layered approach that prioritizes the most disruptive symptoms first. Treatment typically combines cognitive behavioral therapy (CBT), medication like SSRIs or SNRIs, and ongoing reassessment. Because anxiety disorders often overlap, care is flexible and evolves based on symptom changes, patient goals, and treatment response.
Key Takeaways
- Around 60% of people with one anxiety disorder have at least one additional anxiety or depressive diagnosis, making overlap common.¹
- Initial assessments focus on symptom patterns, severity, and co-occurring conditions like depression, trauma, or sleep issues.²
- Clinicians prioritize treating the most disruptive symptoms first, such as panic attacks, severe anxiety, or depression.²
- Cognitive behavioral therapy (CBT) is often central because its core skills apply across multiple anxiety disorders.³
- SSRIs and SNRIs are first-line medications that can treat several anxiety disorders simultaneously.²
- Collaborative care models show better outcomes, with 63.66% response rates vs 44.68% in standard care.³
- Treatment plans evolve over time as symptoms shift and patient needs change.¹
- Nearly 39.1% of adults with moderate to severe anxiety symptoms receive no treatment, highlighting the need for ongoing care.⁴
Why Anxiety Disorders Often Overlap
Anxiety does not usually come alone. Prevalence data has found that 60% of people with one anxiety disorder had at least one additional anxiety or depressive diagnosis, and 27% had three or more.
Conditions like generalized anxiety, panic disorder, social anxiety, and phobia-related fears tend to share roots. Avoidance, chronic worry, and hyperarousal show up across several diagnoses at the same time. Sleep problems, depression, trauma symptoms, and substance use can layer on top.
In practice, clinicians are rarely treating one clean condition. They are navigating a cluster of overlapping symptoms.
What Clinicians Look for During the First Assessment
A first appointment is less about labeling and more about understanding. Clinicians start by asking where the distress is coming from: constant worry, panic episodes, avoidance of social situations, trauma reminders, or physical symptoms without a medical cause.
From there, the picture gets wider. A thorough assessment screens for depression, sleep disruption, substance use, ADHD, trauma history, and any medical conditions or medications that can produce anxiety-like symptoms.
Anxiety disorders can be persistent and likely to worsen over time, meaning clinicians are looking for patterns that have stuck around, not just a rough few weeks. Tools like the GAD-7 help track symptom severity and give both the patient and clinician a baseline to work from, though a screening score alone is not a diagnosis. Therapy cannot begin in the right direction without that kind of foundation.
How Clinicians Decide What to Treat First
Not everything gets treated at once. Most clinicians prioritize the symptoms causing the most disruption: lost sleep, inability to work, withdrawal from daily life, or safety concerns. If panic attacks are the loudest issue, that may come first. If depression is pulling the whole picture down, it often needs early attention because it affects how well any anxiety treatment will take hold.
Patient goals also matter. What does the person want to feel or do that they cannot right now? A clinician who skips that question may build a plan the patient will not follow through on.
Why CBT Is Often Central to Anxiety Treatment
Therapy shows up early and often in anxiety care, and cognitive behavioral therapy is typically at the center of it. CBT works by helping people recognize patterns of anxious thinking and avoidance and respond differently. It is active work, not just talking through feelings, but practicing responses, testing assumptions, and gradually facing feared situations.
When multiple anxiety disorders are present, CBT is especially practical because many of its core skills transfer across conditions. Cognitive restructuring and exposure work apply to panic, social anxiety, and generalized worry alike. Exposure-based work tends to produce the clearest outcomes because it targets avoidance directly, and avoidance is what keeps anxiety going.
When Psychiatric Medication Becomes Part of the Plan
Psychiatry has a clear role when symptoms are moderate to severe, persistent, or affecting multiple areas of life at once. The American Psychiatric Association identifies SSRIs as a first-line medication option for panic disorder, generalized anxiety disorder, agoraphobia, and social anxiety disorder. That cross-condition coverage matters when more than one disorder is present.
Psychiatric treatment with SSRIs or SNRIs does not replace therapy. It shifts the baseline, reducing physical symptom intensity and lowering reactivity, which makes the cognitive and behavioral work in therapy more accessible. Some patients use medication as a bridge while they build skills. Others stay on it long-term. Benzodiazepines sometimes come up, but the APA notes their habit-forming potential means they are generally a short-term option.
How Layered Treatment Works in Real Life
The CALM trial is one of the best real-world examples of anxiety treatment working across multiple diagnoses. The study enrolled 1,004 adults across 17 primary care clinics, many with combinations of panic disorder, GAD, social anxiety disorder, and PTSD. Patients could choose CBT, medication, or both, supported by care managers and web-based symptom monitoring.
At 12 months, response was 63.66% in collaborative care versus 44.68% in usual care. Remission followed a similar gap. The model worked because it was built around each patient’s symptom combination and preferences, not a single protocol applied to everyone.
A follow-up analysis by Craske et al. added useful nuance: Broad psychiatric treatment helped across several conditions, but some comorbid symptoms, particularly social anxiety as a secondary diagnosis, still needed more targeted attention. That finding reflects what clinicians already work with. Flexible care helps. It does not always resolve everything equally.
Therapy does not always wrap up when symptoms stabilize. Booster sessions, relapse prevention planning, and medication review are all part of what long-term care looks like. Symptoms can shift, and a condition that felt resolved can become active again during major stress or life changes.
The 2024 NSDUH data brief from SAMHSA found that 39.1% of adults with moderate or severe GAD symptoms received no mental health services in the past year, many without recognizing a need. That gap matters, and it reinforces why ongoing engagement and honest communication about expectations are part of good anxiety treatment.
| Treatment Type | How It Works | Best For | Strength Across Multiple Disorders |
|---|---|---|---|
| CBT (Cognitive Behavioral Therapy) | Identifies and restructures anxious thought patterns while reducing avoidance through exposure techniques. | Generalized anxiety, panic disorder, social anxiety, phobias | Highly transferable skills that apply across most anxiety disorders |
| EMDR (Eye Movement Desensitization and Reprocessing) | Uses bilateral stimulation to help the brain reprocess distressing memories and reduce emotional intensity. | Trauma-related anxiety, PTSD, persistent emotional triggers | Targets root causes of anxiety when trauma is a contributing factor |
| Medication (SSRIs / SNRIs) | Regulates neurotransmitters to reduce overall anxiety, mood instability, and physical symptoms. | Moderate to severe anxiety, multiple overlapping conditions | Broad symptom relief across multiple anxiety disorders at once |
| Collaborative / Integrated Care | Combines therapy, medication, and care coordination with ongoing monitoring and adjustments. | Complex or comorbid anxiety presentations | Flexible and personalized approach that adapts to evolving symptoms |
What Patients Can Expect From a Customized Treatment Plan
The honest answer is that the plan will evolve. A diagnosis may shift as more information comes in. Therapy may start with one focus and move to another as symptoms change. Medication may need adjusting. Progress is rarely linear, and that is expected, not a sign that treatment is failing.
What a well-built plan provides is structure around that uncertainty. Regular check-ins, symptom tracking, and clear coordination between a prescriber and therapist when both are involved. Patients navigating more than one anxiety disorder at once benefit from that kind of integration because there are more variables in motion.
At Zeam, we build our care around exactly this kind of layered approach. Our team in Sacramento, Folsom, and Roseville offers therapy, including CBT and EMDR, alongside medication management, with specialty options like TMS and ketamine treatment available when needed. If you are dealing with overlapping anxiety symptoms and want a plan that fits your actual situation, contact us today to schedule a consultation.
Citations
- Anxiety Comorbidity Research (PMC): https://pmc.ncbi.nlm.nih.gov/articles/PMC4931606/
- American Psychiatric Association – Anxiety Disorders Overview: https://www.psychiatry.org/patients-families/anxiety-disorders
- CALM Trial & Collaborative Care Outcomes (JAMA / JAMA Psychiatry):
https://jamanetwork.com/journals/jama/fullarticle/185888
https://jamanetwork.com/journals/jamapsychiatry/fullarticle/211217 - SAMHSA NSDUH Data Brief (2024): https://www.samhsa.gov/data/sites/default/files/reports/rpt56935/2024-nsduh-data-brief-gad-symptoms.pdf