Starting a new treatment is rarely a simple yes. When medications have fallen short, and someone mentions TMS therapy, it’s natural to pause, to wonder what it involves, whether it’s right for you, and what happens if it doesn’t work.
That hesitation is worth taking seriously. This article looks at how clinicians sit with patients in that uncertainty: the concerns that come up most, how providers address them, and where TMS therapy fits within a larger mental health plan.
Quick Answer Summary
Clinicians approach patients who are unsure about TMS therapy by addressing concerns around safety, effectiveness, and what treatment involves in a clear, supportive way. They use plain language, walk through the treatment process, and incorporate shared decision-making to help patients feel informed and comfortable. TMS is typically introduced as part of a broader psychiatric care plan, especially for individuals who have not responded to medication. Patients are encouraged to explore their readiness without pressure, ensuring that any decision is aligned with their needs and preferences.
Normalizing the Hesitation
Clinicians who discuss TMS therapy regularly will tell you this upfront: Hesitation is expected. It’s not a red flag. It usually means a patient is paying close attention.
Good providers create space for those questions without rushing past them. They want to know what specifically feels uncertain.
- Is it the technology?
- The time commitment?
- A previous treatment experience that went badly?
The concern behind the hesitation matters, and it shapes where the conversation goes. Sitting with doubt isn’t a detour from care. It’s part of it.
Common Patient Concerns About TMS
A few questions come up almost every time a patient is introduced to TMS therapy. Clinicians have heard them all, and they take each one seriously.
“Is it safe?”
Safety is usually the first thing people want to know. The National Institute of Mental Health describes TMS as a targeted magnetic pulse delivered in a clinical setting without surgery, with no anesthesia, and patients fully awake. A 2025 consensus review from three major neuropsychiatric organizations screened nearly 2,400 studies and concluded TMS has broad evidence for both safety and effectiveness.
“Will it hurt?”
Most patients describe a tapping or clicking sensation on the scalp. It feels strange at first, but it isn’t painful for most people. Clinicians can adjust the intensity early in treatment, and you can flag discomfort at any point during a session.
“What if it doesn’t work?”
No provider can promise results. But a 2025 review in the American Journal of Psychiatry found roughly half of patients with major depressive disorder had a clinically meaningful response to rTMS. That number means something, especially if what you’ve been doing hasn’t moved the needle.
“I’ve tried so many things already.”
Treatment fatigue is real. For patients who’ve been through multiple medication trials, trying something else can feel exhausting before it starts. A 2024 AJP commentary found rTMS more effective at reducing depressive symptoms than switching antidepressants in people who hadn’t responded to two or more prior medications. TMS therapy works through a different mechanism than medication entirely, which is part of why it can succeed where other approaches haven’t.
How Clinicians Educate Without Overwhelming
There’s a difference between giving someone information and helping them actually understand something. Clinicians working with hesitant patients are deliberate about that gap.
Plain language matters. Providers introducing depression treatment options tend to avoid unnecessary jargon, not because patients can’t handle complexity, but because it gets in the way.
Visual aids, short videos, and written materials to review at home all help. Nobody should feel like they must absorb everything in one appointment.
Addressing Fear of the Unknown
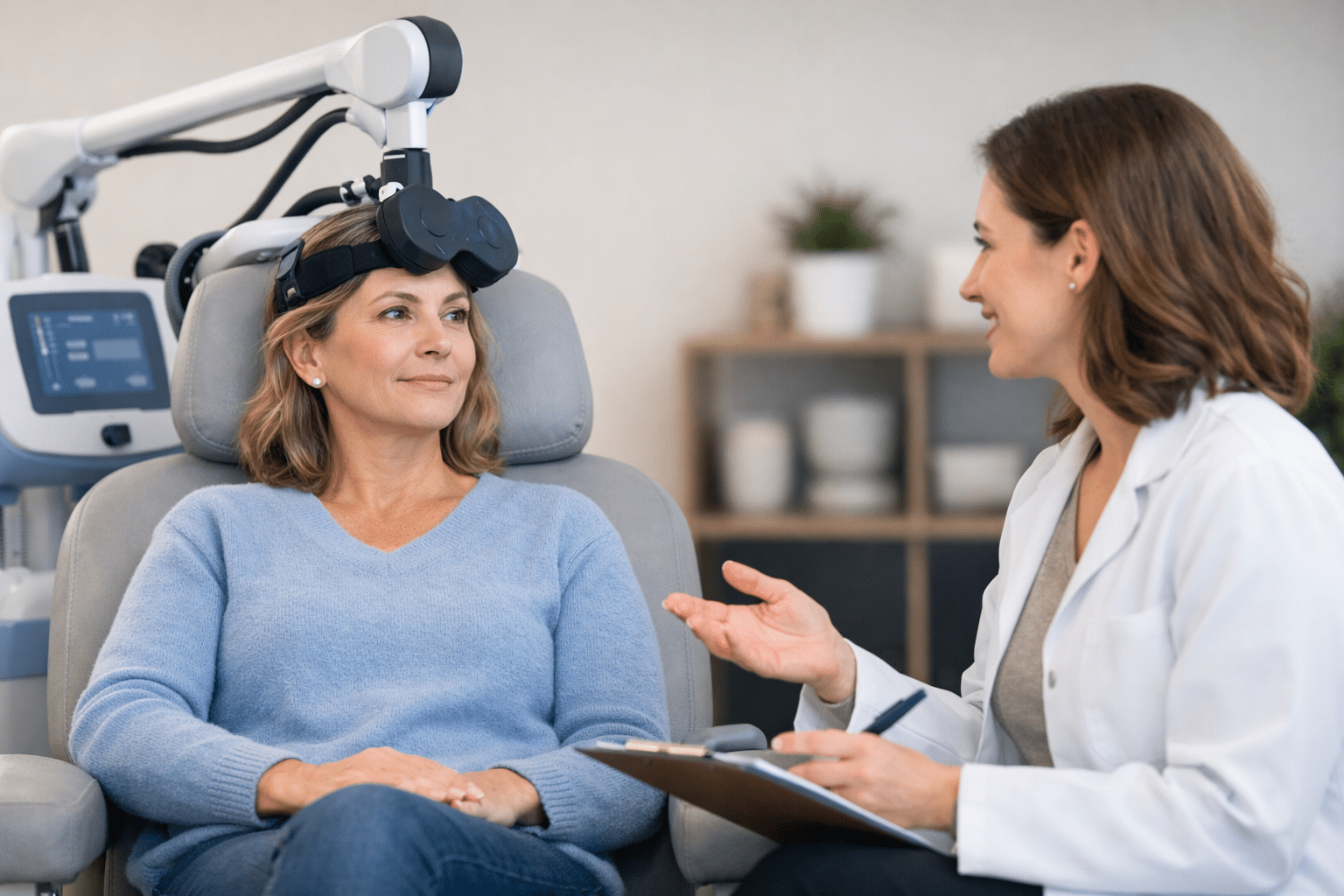
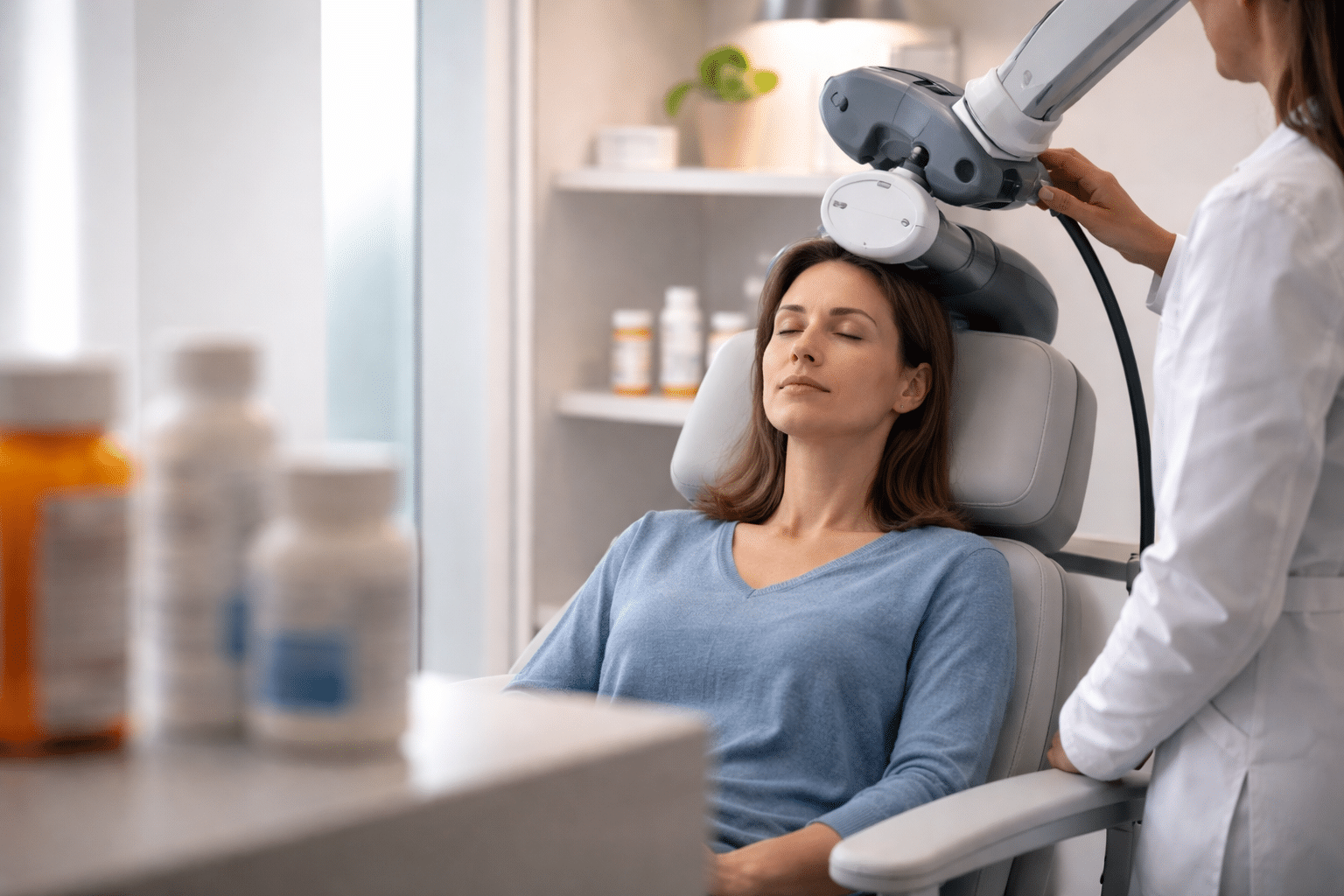
A lot of anxiety about TMS therapy comes from not knowing what a session looks like. Walking through the logistics helps more than almost anything else.
You sit in a chair, fully awake. A clinician positions the device near your head. You hear a clicking sound and feel tapping on your scalp. Sessions typically run between three and forty minutes, depending on the protocol. Afterward, you drive yourself home, no recovery period, no grogginess.
The full course usually runs five days a week for four to six weeks, with some accelerated protocols working faster. A clinical team is present at every session, so concerns can be raised in real time, not weeks later at a follow-up.
The Conversation: Exploring Readiness
Good clinicians ask before they recommend. Open-ended questions, such as “What feels most concerning to you?” create room for patients to say what they’re actually wrestling with.
The VA/DoD Major Depressive Disorder clinical guideline describes this as measurement-based care: using prior treatment history, structured assessments, and shared discussion to validate a patient’s experience and make them an active partner in the process.
- What has worked?
- What caused side effects?
- What does this person actually want their life to look like?
These answers shape whether TMS therapy is even the right conversation to be having.
TMS Within the Broader Psychiatric Treatment Plan
TMS is rarely presented as a last resort, and it’s not a replacement for everything else in a psychiatric treatment plan. It sits alongside therapy, medication management, and lifestyle support, not instead of them.
The VA Community Care clinical determination for TMS outlines what’s typically in place before TMS is recommended: at least moderate depression, a prior medication trial that hasn’t produced adequate results, or documented difficulty tolerating side effects. It enters the conversation as a structured next step, not a random pivot. Choosing to add it doesn’t mean walking away from what’s already been helping.
When Patients Decide to Wait or Decline
Sometimes a patient hears everything and says not now. That’s a legitimate answer. Pushing someone toward a depression treatment they’re not ready for doesn’t produce better outcomes. It leads to dropouts and patients who stop showing up.
When someone decides to wait, providers continue supporting them through other means while leaving the door open. The goal was never persuasion. It was giving someone what they needed to make a choice that felt like theirs.
From Uncertainty to Clarity: Making the Choice That’s Right for You
Hesitation about starting TMS therapy isn’t a sign that you’re not ready to get better. It’s a sign you’re taking the decision seriously, which is exactly what good clinicians are hoping for when they sit down with you.
At Zeam, that conversation starts with listening, not a pitch. We want to know your history, what’s been tried, what hasn’t landed, and what matters to you before anything gets recommended.
If TMS therapy is something you’re turning over in your mind but aren’t sure about yet, reach out. Schedule a consultation, and let’s figure out together whether depression treatment with TMS makes sense for where you are right now.
Key Takeaways
- Hesitation about TMS therapy is normal – Clinicians expect patients to have questions and concerns, and they treat hesitation as part of the decision-making process rather than a barrier to care.
- Safety and effectiveness are well supported – TMS is a non-invasive brain stimulation therapy delivered without anesthesia, and large-scale research supports both its safety and effectiveness in treating depression.¹²
- Common concerns are addressed directly – Patients often ask about safety, discomfort, and effectiveness. Clinicians provide clear answers, emphasizing realistic expectations rather than guarantees.
- TMS works differently than medication – For patients who have not responded to antidepressants, TMS offers a different mechanism of action, which may lead to meaningful improvement where medications have not helped.³
- Education is delivered in a patient-friendly way – Clinicians use plain language, visual aids, and step-by-step explanations to help patients understand what to expect without feeling overwhelmed.
- Shared decision-making is central to care – Treatment decisions are guided by patient history, preferences, and structured assessments, aligning with measurement-based care principles.⁵
- TMS is part of a broader treatment plan – It is typically integrated alongside therapy, medication management, and lifestyle interventions rather than used in isolation.⁶
- Choosing to wait is a valid option – Patients are not pressured into treatment. Clinicians support ongoing care while allowing space for patients to decide when they are ready.
Citations
- National Institute of Mental Health. Brain Stimulation Therapies.
https://www.nimh.nih.gov/health/topics/brain-stimulation-therapies/brain-stimulation-therapies - Consensus review on TMS safety and effectiveness.
https://www.sciencedirect.com/science/article/pii/S1388245724003766 - American Journal of Psychiatry. Effectiveness of rTMS in depression treatment.
https://www.psychiatryonline.org/doi/10.1176/appi.ajp.20240859 - American Journal of Psychiatry commentary on treatment-resistant depression and rTMS.
https://psychiatryonline.org/doi/full/10.1176/appi.ajp.20230556 - VA/DoD Clinical Practice Guideline for Major Depressive Disorder.
https://www.healthquality.va.gov/guidelines/MH/mdd/VADoDMDDCPG_ProviderSummary_Final_508_updated.pdf - VA Community Care Clinical Determination for TMS.
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00026.pdf