For most people diagnosed with depression, the first step is a prescription. Antidepressants are the standard for depression treatment, and for many patients, they work. But not everyone responds the same way, and some people cycle through medications for months without real relief. TMS therapy offers a different path as it works on a fundamentally different mechanism.
This article explains what sets TMS therapy for depression apart from traditional approaches, what treatment looks like, and why some patients end up here instead of or alongside more familiar options.
Quick Answer Summary
TMS therapy differs from traditional depression treatment by directly stimulating targeted brain regions using magnetic pulses rather than altering brain chemistry through medication. Unlike antidepressants, which can take weeks to work and may cause systemic side effects, TMS offers a non-invasive, localized treatment with minimal side effects and no recovery time. It is typically recommended for patients who have not responded to medication or cannot tolerate its side effects, and it is integrated into a broader mental health care plan.
Traditional Depression Treatment
Most depression care begins with medication, and there is good reason for that. SSRIs and SNRIs have decades of research behind them and help a meaningful number of people by adjusting how the brain uses chemical messengers like serotonin and norepinephrine.
The challenge is time. According to the National Institute of Mental Health, antidepressants typically take four to eight weeks to produce their full effect, and sleep, appetite, and energy often improve before mood does. That waiting period is hard for someone already in a depressive episode.
Side effects, including weight changes, reduced libido, and gastrointestinal discomfort, add another layer. They are common enough that some patients stop medication before it has a chance to help. And according to clinical determinations from the U.S. Department of Veterans Affairs, roughly two-thirds of people do not get adequate relief from their first antidepressant. Traditional psychiatric treatment helps many, but it leaves a real gap.
What Is TMS Therapy?
Unlike medication, TMS therapy works by sending magnetic pulses directly into the brain. The main target is the left dorsolateral prefrontal cortex, a region that often runs underactive in people living with depression and plays a direct role in mood regulation.
A 2024 neuroimaging study highlighted by the National Institute of Mental Health found that rTMS can also reach deeper brain areas tied to sadness and anxiety through their surface connections, a more layered mechanism than it might first appear.
Where antidepressants alter brain chemistry throughout the body, TMS works on a defined circuit. No anesthesia, electricity, or systemic effect. That is what makes TMS therapy for depression a fundamentally different kind of intervention.
How TMS Therapy Differs From Traditional Depression Treatment
Non-Systemic, No Medication
One of the most practical differences between TMS and traditional treatment is that TMS stays local. Medications travel through the bloodstream and affect the whole body, which is why antidepressants can produce side effects that have nothing to do with mood.
TMS does not work that way. The magnetic pulses target a specific part of the brain. There is no pill to swallow, nothing entering the bloodstream, and no systemic effect to manage. Most patients experience some scalp discomfort or a mild headache during the early sessions, but the kind of side effect profile associated with depression treatment via medication simply does not apply here.
Patients stay awake throughout and drive themselves home after each session. No sedation, no recovery period, no weeks of uncertainty before knowing whether something is working.
Treatment Experience
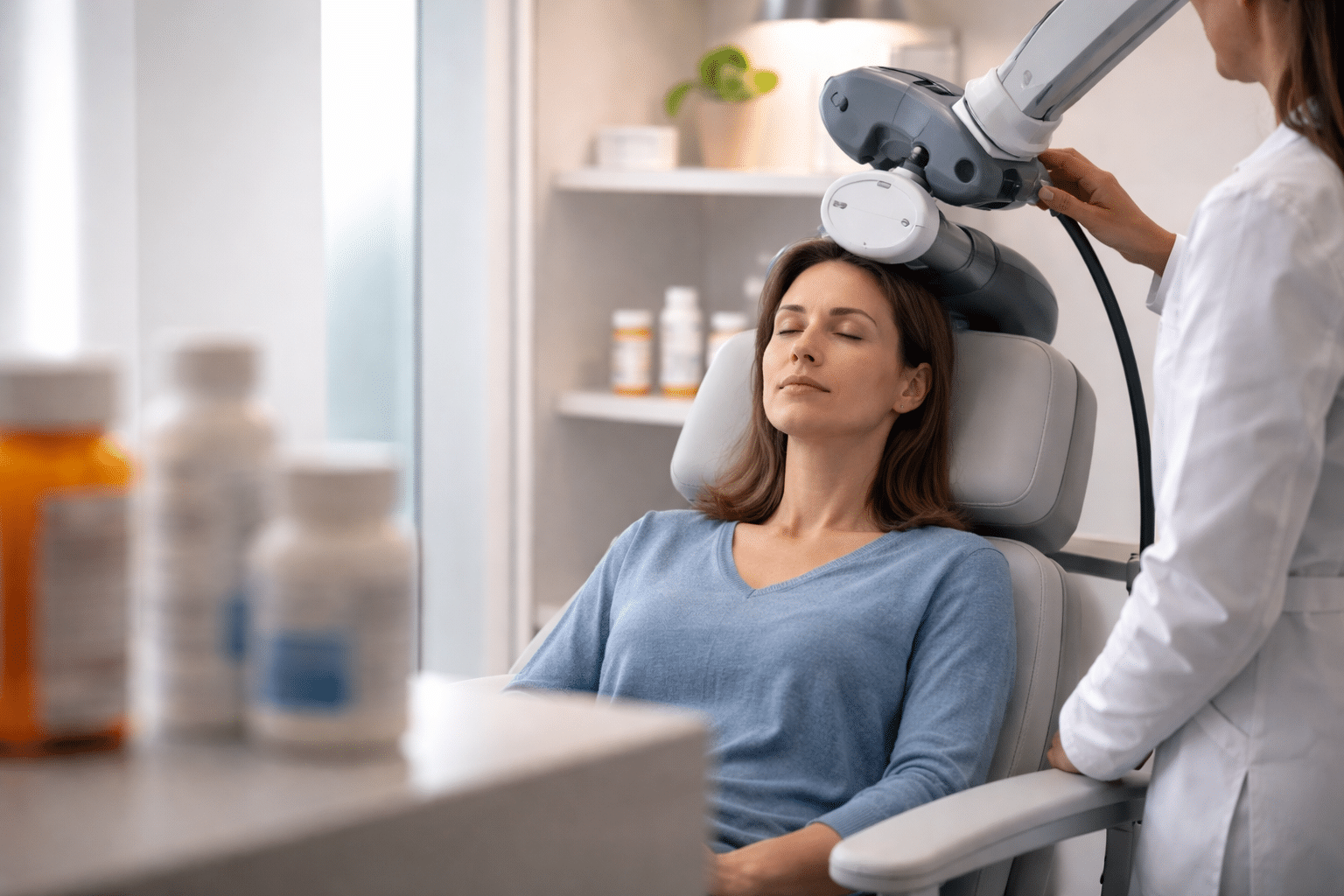
The experience of receiving TMS therapy is unlike most things in mental health care. A patient sits in a reclined chair, a magnetic coil is placed against the scalp, and the device delivers pulses that feel like a rhythmic tapping sensation. Sessions run 20 to 40 minutes.
A standard course runs Monday through Friday for four to six weeks. That structure is deliberate, as consistent stimulation is what drives the neurological changes. A 2025 consensus review by the National Network of Depression Centers and Clinical TMS Society, covering nearly 2,400 published abstracts and manuscripts, found that newer protocols like intermittent theta burst stimulation are non-inferior to standard rTMS and can be completed faster.
Compare that to a daily pill, month-long titration periods, and side effect adjustments. The experience of psychiatric treatment through TMS is structured and time-limited in a way that medication management rarely is.
Who TMS Is For
TMS is not usually the first thing a clinician reaches for. It typically enters the picture after standard approaches have been tried.
The FDA has cleared TMS devices specifically for adults with major depressive disorder who have not responded adequately to prior antidepressant medication in the current episode, which is the patient group that faces the longest and most frustrating treatment journeys. The FDA clearance summary for the Ampa One System describes targeted stimulation of the left dorsolateral prefrontal cortex and dorsomedial prefrontal cortex, depending on the protocol.
Some patients seek TMS therapy for depression because they have not found adequate relief from medication. Others arrive because they cannot tolerate the side effects, even when the medication technically “works,” living with the consequences can be its own problem.
For patients who need something more intensive than medication but want an alternative to electroconvulsive therapy, TMS offers a less invasive middle option. The VA’s clinical guidance describes TMS in exactly this role: a step forward for patients who cannot tolerate or do not want ECT.
In March 2024, the National Institute of Mental Health also reported that the FDA cleared a rapid-acting form of rTMS for treatment-resistant depression, and separately cleared rTMS as an adjunctive depression treatment for adolescents aged 15 and older. The patient population for TMS is growing.
| Category | TMS Therapy | Traditional Depression Treatment |
|---|---|---|
| How it works | Uses targeted magnetic pulses to stimulate specific brain regions involved in mood regulation. | Typically uses medications like SSRIs or SNRIs to alter neurotransmitter activity throughout the body. |
| Systemic effects | Localized treatment with no medication entering the bloodstream. | Systemic treatment that can affect multiple body systems. |
| Common side effects | Usually mild scalp discomfort or headache early in treatment. | May include nausea, fatigue, weight changes, reduced libido, or gastrointestinal issues. |
| Time to treatment course | Structured sessions, usually five days a week for four to six weeks. | Often involves daily medication use with dose adjustments over a longer timeline. |
| During treatment | Patient remains awake, alert, and can drive home afterward. | Medication is taken at home, but side effects and response may take time to evaluate. |
| Best fit | Often considered for patients who have not responded to antidepressants or cannot tolerate side effects. | Common first-line treatment for many patients starting depression care. |
| Approach | Non-invasive, device-based brain stimulation. | Medication-based treatment aimed at chemical signaling pathways. |
| Role in care plan | Often integrated with therapy, psychiatry, and lifestyle support. | Also commonly combined with therapy and ongoing psychiatric monitoring. |
What Patients Should Know Before Considering TMS
Not everyone qualifies. Patients with certain metal implants in or near the skull, such as cochlear implants and some aneurysm clips, are typically excluded, and a history of seizure disorders warrants careful evaluation before proceeding with TMS therapy.
On the cost side, it is less daunting than most people assume. TMS is FDA-approved, and the majority of major insurance plans cover it, including Medicare, when treatment-resistant criteria are met. Worth confirming early, but coverage is fairly common.
Commitment matters. Results from TMS tend to accumulate across the treatment course. Skipping sessions or stopping early can limit outcomes, so patients who follow through consistently see the strongest results.
A New Option When Traditional Paths Fall Short
Depression treatment has evolved considerably. For patients who have struggled with medication, whether because of insufficient response, side effects, or both, TMS therapy represents something genuinely different: a non-invasive, brain-targeted, evidence-based approach that works through a mechanism distinct from anything in a pill bottle. It does not work for everyone, but it has a clear, documented benefit for a meaningful portion of people who had started to think nothing would help.
Finding the right depression treatment takes time, and not every path looks the same. At Zeam, we work with patients in Sacramento, Folsom, and Roseville who are ready to explore options beyond what they’ve already tried. TMS therapy is one of those options, and for the right candidate, it can make a real difference. Contact us to learn whether TMS therapy for depression fits where you are right now.
Key Takeaways
- Traditional treatments rely on medication – Antidepressants like SSRIs and SNRIs adjust neurotransmitters such as serotonin and norepinephrine, but can take weeks to show full effects and may cause side effects.¹
- Many patients do not respond to first-line treatments – Clinical data shows that a significant portion of patients do not achieve adequate relief from their first antidepressant, creating a need for alternative approaches.²
- TMS works through a different mechanism – TMS uses targeted magnetic pulses to stimulate specific brain regions involved in mood regulation, rather than affecting the entire body through medication.⁶
- It is non-invasive and non-systemic – Unlike medications, TMS does not enter the bloodstream and does not produce systemic side effects, making it an appealing option for patients sensitive to medication.
- Treatment is structured and time-limited – TMS therapy typically involves daily sessions over several weeks, with each session lasting 20 to 40 minutes and no downtime afterward.
- It is designed for treatment-resistant depression – TMS is FDA-cleared for patients who have not responded adequately to antidepressant medication, offering a next-step option in care.⁵
- Research supports both safety and effectiveness – Large-scale reviews and clinical studies confirm that TMS is a safe and effective treatment for depression, with ongoing advancements improving efficiency and accessibility.⁴
- It fits within a broader treatment plan – TMS is often combined with therapy, medication management, and lifestyle changes as part of a comprehensive psychiatric care approach.
Citations
- National Institute of Mental Health. Mental Health Medications.
https://www.nimh.nih.gov/health/topics/mental-health-medications - VA Community Care Clinical Determination for TMS.
https://www.va.gov/COMMUNITYCARE/docs/providers/CDI/IVC-CDI-00026.pdf - National Institute of Mental Health. Noninvasively stimulating deep brain areas to treat depression.
https://www.nimh.nih.gov/news/science-updates/2024/noninvasively-stimulating-deep-brain-areas-to-treat-depression-symptoms - Consensus review on TMS safety and effectiveness.
https://www.sciencedirect.com/science/article/pii/S1388245724003766 - FDA Clearance Summary for TMS device (Ampa One System).
https://www.accessdata.fda.gov/cdrh_docs/pdf24/K243319.pdf - National Institute of Mental Health. Brain Stimulation Therapies.
https://www.nimh.nih.gov/health/topics/brain-stimulation-therapies/brain-stimulation-therapies